Labor and Delivery Introduction
One of the most important steps women can take toward a positive labor and delivery experience is to learn about it. When various aspects of childbirth are explained in more detail, women can understand the process much better and feel more in control.
First, women should expect to start labor within a four-week time frame – with their due date at the center. When women expect to start labor on or within just a few days of their due date, this can set them up for inevitable frustration.
The least amount of time that is considered the most accurate for the start of labor is between 38 and 42 weeks; based on how due dates are calculated, no part of this time is technically "early" or "late" unless labor falls outside this range.
The instant recognition of the start of labor is not currently possible for most women. Most of the time, this is only recognized after the fact. Therefore, the best and fastest way to determine if a woman is truly in labor is to time contractions as soon as they begin, to established a baseline toward progression.
Labor is separated into 4 stages; learning about each stage one at a time can help women better comprehend what is expected during each stage (although significant overlap can occur).
Women should read as much as they can about the labor and delivery process and direct all questions and concerns they have to their HCP. It is important for women to understand they have many options for how they would like to labor and deliver their baby. However, labor is incredibly unpredictable; women should remain flexible, keep an open mind, and read more below to learn when and why HCPs may make certain recommendations.
Background
Learning about labor and delivery for the first time can be very overwhelming; even normal, uncomplicated labors have many unknowns and women may be asked to make numerous decisions as they progress toward delivery.
Labor and delivery occurs in stages; women may find it very helpful to learn about each stage, one at a time. While interventions and unexpected events can occur at any stage, labor generally occurs in the following order:
Stage 1: Start of contractions to full dilation
Stage 2: Pushing to delivery
Stage 3: Placenta removal
Stage 4: Immediate recovery
From an educational standpoint, there may also be a "pre-stage"; an early "stage" of physiological events, signs, symptoms, or actions that occur (or should occur) just prior to the start of labor. Although not all of these factors are recognized by all women, when they are, they can help women physically, mentally, and emotionally better prepare for labor.
Further, learning more about these "Stage 0" aspects can help women better understand what their body is doing, why some women start labor earlier or later than others, what occurs during labor, and why certain options are available and when.
Stage 0 ("Before" Labor)
Due Date and Gestation: Women should remember near term that a "due date" only exists to mark a period of four weeks, which is the least amount of time that can be considered the most accurate as to when a woman will go into labor. Women who deliver two weeks prior or two weeks after their "due dates" are not "early" or "late" (just before or after the due date they were given).
However, preterm is defined as less than 37 weeks, and postterm is defined as more than 42 weeks (read more).
Fear of Childbirth: A fear of labor is common, and this may increase and reach a peak as women get closer to term. An intense or extreme fear of labor can affect the labor process by either lengthening it or increasing a woman's perception of pain.
Although not much evidence-based information exists on management techniques, it appears the best "treatment" is valid and accurate information from reliable sources regarding the labor and delivery process, as well as pregnancy itself.
Women need to share their fears and concerns with their HCP, who can help them process information related to their concerns, as well as provide the resources necessary to have a positive pregnancy and birth experience (read more).

Birth Plan: Numerous websites offer helpful downloadable birth plans that have dozens of questions and categories of choices, but these can be very overwhelming. Women should try to learn what they can about pregnancy and labor and delivery first, prior to completing any of these guides.
Once a woman determines how she really feels about a topic, has discussions with her HCP, and learns the options available to her at her chosen health care facility, she can begin to narrow down her preferences – that’s when those downloadable options are likely the most helpful (read more).
Prostaglandins: Prostaglandins are hormones that affect various aspects of the reproductive system. Near term, a woman's body releases and uses prostaglandins to begin ripening the cervix.
If a woman does not make enough prostaglandins, or an induction is required and the woman’s cervix is not yet favorable, pharmaceutical prostaglandins and mechanical methods can be used. The goal is to get the cervix ripe enough to potentially start contractions and further progress dilation and effacement.
Starting Labor Naturally: These methods include consuming certain foods or engaging in specific activities toward the end of pregnancy that may release natural prostaglandins or oxytocin with the goal of initiating labor. Unfortunately, based on current evidence, there are few methods that appear to have any lasting effect.
While some methods do force the body to release natural oxytocin or prostaglandins, which may cause minor contractions, it is unlikely these methods produce an effect on a scale that is long or strong enough to induce labor.
Further, some of these methods are based on theories that intestinal distress (diarrhea, cramping, indigestion) can cause uterine contractions; therefore, women may experience distressing or even harmful side effects (read more).

Membrane Sweep: A membrane or cervical sweep (or strip) is a “natural” technique used to potentially initiate the start of labor through forced induction of prostaglandins.
The procedure involves an HCP placing a finger through the cervix to separate the membranes from the uterine wall and internal os of the cervix. It can be effective at starting contractions within 48 hours in about 1 in 8 women and is not associated with significant risks or complications (read more).
Mucus Plug: The cervical mucus plug forms early in pregnancy to create an impermeable and immunological barrier from potentially harmful bacteria located in the lower genital tract. It is expected that when formed properly, this plug can protect the amniotic cavity from infection. As the cervix ripens and softens, the plug will fall out.
The mucus plug falls out in some women sometime between 37 and 42 weeks of pregnancy, while others lose their plug after labor has already begun; the plug can fall at all at once or gradually, and is therefore not always recognized. While losing the plug prior to contractions is a good sign the cervix is ripening, labor could still be days or weeks away (read more).
It is known, however, that some bacteria can get through the plug, and an estimated 1 in 3 preterm deliveries are thought to occur due to infection that originated in the lower genital tract (learn to recognize signs of infection to possibly prevent preterm labor).
Induction of Labor: For women who need to deliver, but labor has not yet started on its own, induction is recommended. This technique uses medications and/or mechanical methods to initiate or progress cervical ripening, contractions, and dilation and effacement.
Women have various options for induction of labor which are safe, effective, and have many safeguards and specific techniques in place to avoid serious complications.
All women – no matter what their birth plan is – should be aware of the methods and options for induction in the event it is recommended near term or during labor. This way, women have time to understand the process, the methods used, the risks and benefits of each, and have plenty of time to ask their HCP questions (read more).
Stage 1: Start of Labor to Full Dilation
The start of labor becomes official when contractions – whether initiated spontaneously or through induction – become regular, gradually increase in intensity, and lead to cervical change.
Contractions (and Start of Labor): Contractions are the key to determining the start of labor, and recognizing a true, gradual pattern as early as possible can help women feel less uncertain about when to go to the hospital/birthing center (read more).
Eating During Labor: Some women may be in this first stage for hours; women can get tired and lose energy quickly – prior to pushing. Most hospitals around the country have a standard policy of fasting (no eating) during labor. Clear liquids are usually allowed, and most women may also receive intravenous fluids.
However, current evidence indicates that fasting itself can cause complications; therefore, some health care facilities and practices have begun allowing women to eat small snacks while in labor. Women need to inquire whether their HCP or facility in which they intend to deliver allows women to eat during labor, or after admission (read more).
Note: Women who have planned/scheduled cesarean sections will need to follow different fasting rules.
Dilation and Effacement: Dilation (10 centimeters) and effacement (100%) must occur before the baby can pass through the birth canal for delivery. With the progression of contractions and the fetal head pressing down onto the cervix, the cervix completes dilation and effacement, and women can begin pushing.
Current research indicates that women dilate at variable rates; therefore, in the absence of fetal and maternal distress, women should be offered time to dilate, prior to augmentation methods by an HCP – unless the woman desires to speed up her labor (read more).
Rupture of Membranes: The rupture of fetal membranes can occur at any point during pregnancy, but usually occurs during labor and near the end of dilation. An amniotomy is the purposeful rupture of membranes by an HCP; this method is often used to speed up (or augment) the progress of labor (read more).
Epidural: An epidural is the most common form of pain medication used by women during labor and delivery; women also have various additional options available, from the type of epidural received to the dosage administered.
Although there are risks associated with the use of an epidural, these are rare, the failure rate is low, and many risk-prevention techniques are in place to avoid complications (read more).
Stage 2: Pushing to Delivery
Pushing: Pushing occurs during the second stage of labor, which is full dilation to delivery. The length of time it can take women to push during this stage is affected by numerous variables. Some women may only need a couple pushes, while other women may need 2 to 3 hours.
In the absence of maternal or fetal distress, women have options regarding when they would like to push, how they want to push, and the position in which they would prefer to push.
There is no single position that has been shown to work best for all women, shorten the duration of labor, or cause the last amount of perineal tearing or trauma. It is therefore recommended that women should be encouraged to choose positions that make them the most comfortable (read more).

Tearing (and Episiotomy): Crowning – the term used for when the widest part of the baby’s head arrives at the vaginal opening – can cause some women to tear through various tissues in the vaginal, perineal, anal, and/or rectal areas (but not always). Most women tear to some degree with their first vaginal delivery, but only a small percentage experience more severe tearing.
An episiotomy – a purposeful incision made about halfway into the perineum – was used routinely until the early 2000s. Today, however, episiotomies are only performed under strict circumstances as almost all evidence completed since its routine use indicates that episiotomies have almost no benefit unless the baby needs to come out as soon as possible (read more).
Prolonged/Protracted Labor: “Failure to progress” is a common concern for pregnant women who wish to avoid a cesarean section. Formally called dystocia, it has been suggested that this term should be renamed to protracted latent phase of labor (first stage – dilation) and prolonged active phase of labor (second stage – pushing), which better reflects current research showing that women labor and dilate at varying rates.
This updated research and more relaxed definition allows for more caution in the diagnosis of a slow labor, and gives women more time to labor down, rest, change positions, feel more in control, and attempt to relax; all with a focus of pushing with each contraction – as long as the baby shows no signs of distress (read more).
Assisted Delivery: Assisted delivery has changed in the last few decades, with more HCPs being trained – and specifically choosing to use – vacuum extraction over forceps. However, research indicates that overall, HCPs are choosing cesarean section over any attempt at assisted delivery during a prolonged pushing stage.
Cesarean section is considered to have higher risks to both mother and baby than assisted delivery, and the American Congress of Obstetricians and Gynecologists is encouraging HCPs to use assisted delivery to lower cesarean section rates. An HCP must be properly trained and comfortable in using various assisted delivery techniques, as both are recommended for very specific purposes in the second stage of labor (read more).
Stage 3: Placenta Removal
After the baby is delivered, the placenta will also be delivered within 5 to 60 minutes depending on whether active or expectant management of the placenta is used. This process is described in more detail under Stages of Labor, including the actual process of what women can expect during each stage from the start of labor, to contractions, and dilation and effacement to vaginal delivery.
Women can also learn about the placenta as an organ here.
Cesarean Delivery
An HCP can determine at any point before or during attempted vaginal delivery that cesarean section may be necessary. The HCP will discuss this with a woman/couple, and they can make a decision regarding the best path forward.
Cesarean Section Overview: Cesarean sections, in which the uterus is surgically cut open to deliver a baby, are commonly performed around the world as both planned and unplanned operations.
Due to changes that can occur suddenly during labor, women planning a vaginal birth need to be aware of information regarding cesarean sections, the procedure, and the risks, in the event the procedure becomes necessary (read more).
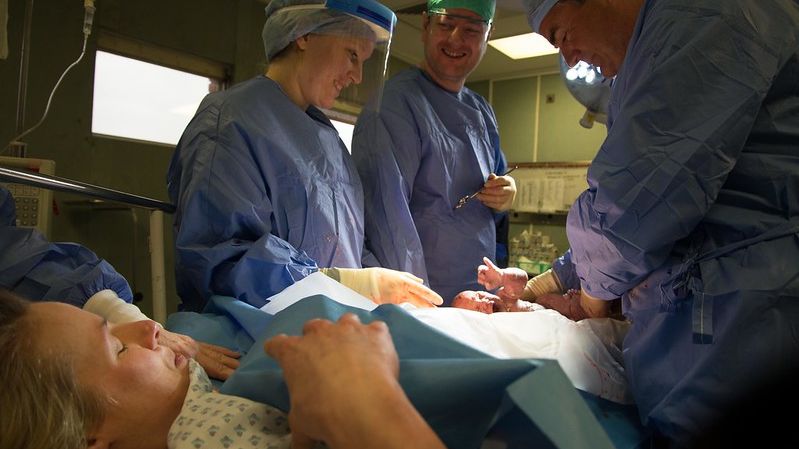
Cesarean Section Procedure: Cesarean section is one of the most performed surgical procedures in the United States, and the procedure itself is done very similarly across all countries. The baby is usually born within the first 10 minutes of the procedure (the first 60 seconds in an emergency). The majority of the procedure occurs after the baby has been born, but as long as there are no complications (which are rare) the mother can still see her baby after delivery.
Stage 4: Immediate Postpartum Recovery
A fourth stage is sometimes added, termed “immediate postpartum care". This stage represents the period of a few hours after expulsion of the placenta when close observation is desirable to avoid or detect postpartum hemorrhage and signs of infection or high blood pressure.
Labor and delivery nurses remain critical resources during this stage, as they help women control bleeding and pain, provide breastfeeding assistance, newborn care, and can offer the entire family mental and emotional support during their hospital stay.

Action
Women should being reading about the different aspects of labor and delivery as soon as they can during their pregnancy. This provides them enough time to process and direct all questions and concerns they have to their HCP and to develop their birth plan.
It is also important for women to understand they have many options for how they would like to labor and deliver their baby. However, labor is incredibly unpredictable; women should remain flexible, keep an open mind, and find an HCP who will do the same (read Types of Healthcare Providers).
Resources
Safe Prevention of the Primary Cesarean Delivery (American College of Obstetricians and Gynecologists)
How to Tell When Labor Begins (American College of Obstetricians and Gynecologists)
Approaches to Limit Intervention During Labor and Birth (American College of Obstetricians and Gynecologists)
Labor Induction (American College of Obstetricians and Gynecologists)
Preterm Labor and Birth (American College of Obstetricians and Gynecologists)
Intrapartum care for healthy women and babies: Information for the Public (U.K. National Institute for Health and Care Excellence)