Types of Health Care Providers

Pregnant women will encounter numerous different types of Health Care Providers (HCP) during their pregnancy, especially at a large practice or university teaching hospital.
It is recommended that women familiarize themselves with the different types, training, education, and responsibilities of each, and then determine the type of care and style that makes women the most comfortable for their pregnancy.
Further, understanding how these positions interact with each other and why women may be introduced to different professionals can help make women more at ease and feel more secure with their entire prenatal, labor and delivery, and postpartum experience.
Background
Outside of emergencies, only OB/GYNs and midwives (and at times, Physician's Assistants) can formally deliver babies. However, Registered Nurses offer unparalleled support and are present at almost all births in a hospital/birthing center. Women may also wish to have a doula present throughout their entire labor to offer emotional and informational support.
Some women may prefer seeing different HCPs to get different perspectives and personalities, as well as to meet the possible individuals who could end up delivering their baby – especially in large practices. Others will prefer the exact opposite and wish to see the same individual at every appointment, and have that individual deliver their baby (although this may be impossible to completely guarantee).

Women need to feel comfortable and completely at ease with their health care team during pregnancy. Women should read Birth Plan and Appointments as addendums to helping them make a decision on whether a certain provider/health care facility is a right fit.
OB/GYNs
Gynecology is the field of medicine concerned with the health of the female reproductive organs. It also overlaps with the fields of endocrinology (hormones), female urology (urinary system) and pelvic oncology (cervical, uterine, ovarian cancers).
Gynecologists do not deliver babies or treat pregnant women, but focus on all other aspects of reproductive health, such as fibroids, urinary tract infections, and endometriosis.
Obstetrician-gynecologists (OB/GYNs) are physicians who possess special knowledge, training, and skills related to the medical and surgical aspects of the female reproductive system as well as pregnancy, labor, delivery, and the immediate postpartum. Some women may also use their OB/GYN as their primary HCP.
After medical school graduation, future OB/GYNs complete residency-training programs focused on health in all stages of pregnancy – usually four years of an accredited, clinically-oriented education. Topics include:
Ultrasonography
Reproductive endocrinology
Infertility
Family planning
Gynecologic surgery/oncology
OB/GYNs in private practice typically run a schedule of office hours (appointments) two to four days a week, surgery one to two days a week, and management of labor and delivery, usually on a rotating basis with other physicians who may be in the same practice. OB/GYNs commonly work very long hours due to the unpredictable nature of labor and delivery.
Maternal-Fetal Medicine Sub-specialist
A maternal-fetal medicine (MFM) subspecialist is an OB/GYN physician who has completed an additional two to three years of education and training regarding high-risk pregnancies, to include those who develop complications during an otherwise normal pregnancy. Possible complications can include bleeding, gestational diabetes, preeclampsia, premature rupture of membranes, preterm labor, and high blood pressure.
Further, in some cases in which OB/GYNs detect a birth defect or other condition with the baby, MFMs may be able to start treatment before birth by providing monitoring, blood transfusions and even surgery, if necessary.
Midwives
Midwives are highly educated, specialized professionals who work alongside OB/GYNs to provide prenatal care – to include labor and delivery. Professional midwives can deliver at homes, hospitals, or birthing centers.
Midwives provide a higher level of continuity for women during their pregnancy, who wish to have:
Only one provider throughout gestation
A stronger relationship with that provider
Higher confidence in knowing the exact provider who will deliver their baby
Midwives follow the general principle of not interfering in different phases of natural delivery (such as using augmentation methods) and avoid using medications or techniques that may be routine with OB/GYNs (unless a woman requests them). This aspect of care can provide a significantly higher positive birthing experience for certain women.
A midwife can (depending on certification):
Perform regular exams
Provide women evidence-based information regarding all aspects of pregnancy
Perform deliveries
Provide postpartum medical and newborn care
Offer breastfeeding assistance
Provide emotional support for the entire family
All midwives who work in birthing centers or hospitals have a relationship with an obstetrician in case of complications; physicians – not midwives – perform cesarean sections.
There are four main types of midwives:
Certified Nurse Midwife
Certified Nurse Midwives (CNMs) are highly trained, have extensive medical backgrounds, and typically hold a Master of Science degree in Nursing. CNMs must pass a national certification exam by the American Midwifery Certification Board (AMCB). Re-certification every 5 years is mandatory.

Certified Midwife
Certified midwives are individuals who have a background in a health-related field other than nursing but graduate from a midwifery education program accredited by the AMCB. CMs take the same national certification examination as CNMs.
All CNMs can prescribe medications; CMs may prescribe medications, but this depends on state law; insurance programs generally cover the costs of CNMs and CMs.
Certified Professional Midwife
Certified Professional Midwives are not required to have a graduate degree, as are CNMs and CMs. They are certified through the North American Registry of Midwives (NARM) rather than the AMCB in skills necessary for maternity care, to include labor and delivery. CPMs generally cannot prescribe medication, but some states may allow minor exceptions.
Most CPMs work in home or birthing center facilities, while most CNMs and CMs work in hospital settings.
Lay/Traditional Midwife
Lay midwife refers to an uncertified or unlicensed midwife who usually has an informal education in labor and delivery rather than a formal education; some states require specific licensing for lay midwives, while others do not.
Physicians Assistant
Physician Assistants (PA) can perform a wide range of outpatient diagnostic and therapeutic procedures, to include obstetrics examinations and the evaluation of gynecological conditions. PAs usually work in a team model with physicians.
PAs can:
Perform annual pap/pelvic and breast exams
Address gynecological complaints (fibroids, cysts, endometriosis)
Provide family planning services
Prescribe medications
Perform deliveries (vaginal only; depends on state and facility); may assist in cesarean sections
Provide prenatal and postpartum care
PAs have a minimum of a master’s degree and have completed a PA program lasting three academic years that includes classroom instruction and more than 2,000 hours of clinical rotations.
Registered Nurses
Labor and Delivery Nurses (LDN) are Registered Nurses who are present at almost all births either in a hospital or birthing center and play a pivotal role in positively affecting a laboring woman’s birth experience. LDNs work alongside OB/GYNs and midwives to care for pregnant women in labor or pregnant women admitted to a hospital due to complications.
LDNs are highly skilled and knowledgeably in all four stages of childbirth: antepartum (during), intrapartum (labor/delivery), postpartum, and neonatal (baby).
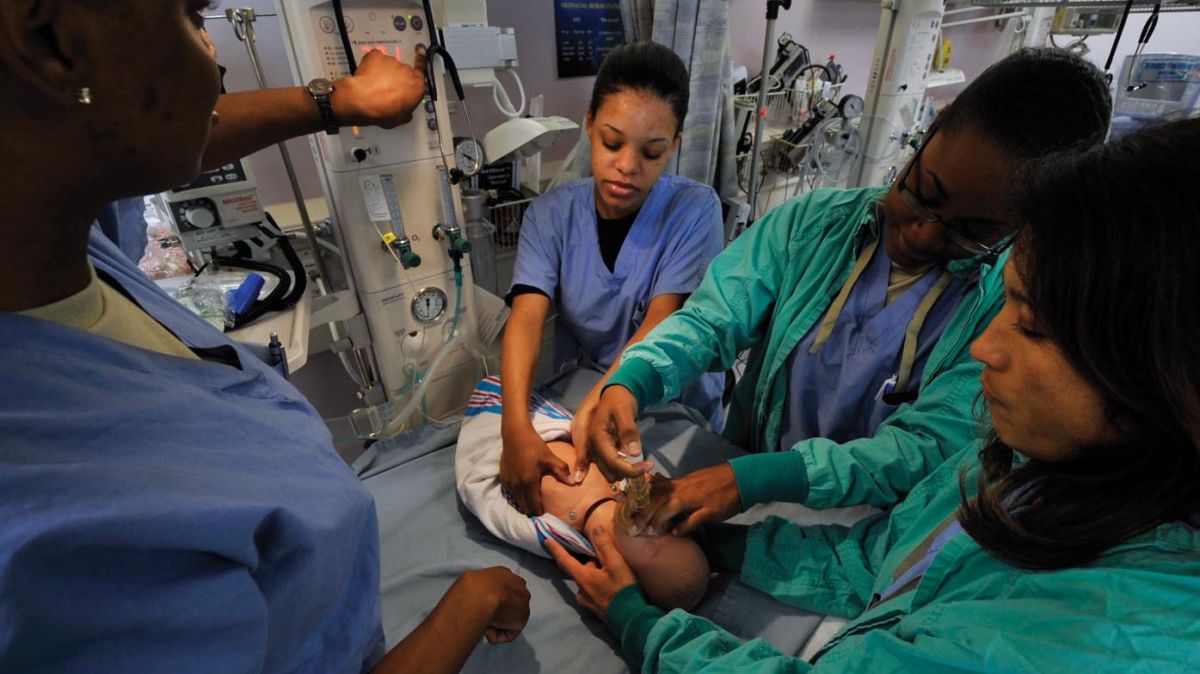
LDNs have years – even decades – of experience that can be invaluable for almost all pregnant women. LDNs know how to answer questions, control the environment, keep things calm, help women through their labor pain, assist women’s partners/support through the process, and comfort and reassure women who are scared or anxious.
LDNs also:
Administer (but not prescribe) medication
Provide direct care and support to women, their partners, and their newborns
Respect women’s wishes, listen to their birthing decisions, offer advice, and act as a communication channel between women and the OB/GYN or midwife.
Monitor fetal and infant health status and provide information to the delivering physician
Interpret contraction and fetal heart rate monitoring and update women on their labor progress
Assist OB/GYNs and midwives with delivery
Help with immediate postpartum/recovery and newborn care
Women can vary in their desire in what they want from an LDN; some women will want more continual support, while others may want more privacy.
LDNs have numerous responsibilities and likely more than one laboring woman simultaneously. LDNs come in and out of rooms when necessary, and often do not have time to remain in the room of any one particular woman – unless the woman is close to pushing, is experiencing complications, or the practice/birthing center is small.
However, despite this, LDNs have a strong impact on pregnant and laboring women, are invaluable in their knowledge and skill set, and tend to form strong bonds with women in their care, especially based on their 12-hour shifts.

An LDN requires an Associate Degree in Nursing or Bachelor of Science in Nursing program. Further, every nurse must pass their state's NCLEX-RN examination for licensure in order to be considered a Registered Nurse. LDNs may also be required to take the Inpatient Obstetric Nursing (RNC-OB) certification after around 24 months of employment.
Nurse Practitioner
A Nurse Practitioner (NP) is an Advanced Practice Registered Nurse (APRN) that has earned either a Master of Science in Nursing (MSN) or a Doctor of Nursing Practice (DNP) and received advanced clinical training beyond their skill set necessary as a Registered Nurse.
NPs provide high-quality care in all communities to include clinics, hospitals, emergency rooms, urgent care sites, private physician or NP practices, nursing homes, schools, colleges, and public health departments.
NPs can:
Order, perform, and interpret diagnostic tests
Diagnose and treat acute and chronic conditions
Prescribe medications
Provide evidence-based information regarding prenatal care
Offer counseling
While an NP can work in an obstetric office and provide prenatal care, NPs do not perform deliveries.
Some states offer NPs full autonomy and to see patients without the supervision of a doctor. However, in other states, although NPs have more authority than RNs, they do need a doctor to sign off on certain medical decisions.
Anesthesiologist
An anesthesiologist performs epidurals and administers the anesthesia necessary prior to a cesarean section or other obstetric/gynecological procedures. An anesthesiologist has 12 to 14 years of education and 12,000 to 16,000 hours of clinical training.
An anesthesiologist will speak to women either before labor, after admission, or during labor to inform women of their pain relief options. Women may also be offered a combination of options.
A Certified Registered Nurse Anesthetist (CRNA) may also perform an epidural.
CRNAs are Advanced Practice Registered Nurses (APRNs) who administer anesthesia and other medications. They also monitor patients who are receiving and later recovering from anesthesia.
CRNAs usually have a Bachelor of Science in Nursing degree, then become a licensed RN and gain a few years of experience during employment. RNs who wish to become CNRAs then get accepted into an accredited nurse anesthesia program (master’s) which can take between 2 and 4 years to complete, followed by a certification exam approved by the National Boards of Certification and Recertification of Nurse Anesthetists (NBCRNA).
Doula
A doula is an individual trained to provide continual physical, emotional, and informational support to women during labor, birth, and in the immediate postpartum period (which doula advocates call the “fourth trimester”).
Doulas focus on individualized emotional and informational support before, during, and after birth and adapt to the needs of one woman at a time during that woman’s own, unique delivery experience. Doulas are a source of constant support/presence during labor and delivery whereas nurses and other HCPs may have numerous responsibilities/women to care for simultaneously.

Doulas are nonmedical professionals that work alongside medical staff to:
Maintain a constant presence at the woman’s side
Serve as the woman’s advocate
Offer laboring/positional techniques to reduce pain
Offer nonjudgmental support
Provide emotional support for a laboring woman
Provide calm during unpredictable labor situations
Give the partner/support individual a break/some rest
Provide women with the confidence necessary to make their own medical decisions
Serve as an intermediary between the woman, her partner, and physician
Although use of doulas remains low in the United States overall, the practice is increasing in recent years due to evidence-based information illustrating the proven benefits to an entire family regarding the birth experience.
In 2014, ACOG and the Society for Maternal-Fetal Medicine found that continuous labor support (such as through the use of a doula) is among “the most effective tools to improve labor and delivery outcomes".
Further, studies examining the impact of continuous support by doulas have reported significant reductions in cesarean births, instrumental (assisted) deliveries, need for oxytocin, and overall shortened durations of labor, along with higher breastfeeding rates.
Properly trained doulas are educated on the birthing process and/or postpartum period and have met the requirements of a rigorous certification program.
The Doulas of North America (DONA) is considered the leader in evidence-based doula training, certification and continuing education. However, the profession is generally unregulated, and most doulas have no prior history, education, or professional experience in the field of health care (but they have a passion for it).
Doulas certified/trained through DONA or other programs can be very effective and beneficial for pregnant women. However, women need to ask their potential doula for their credentials/certification and experience, asking for as much detail as possible until all parties are comfortable.
The cost of a doula varies, but averages between $300 to $1,200; the number of prenatal visits and postpartum assistance may also vary by price and by doula. As of May 2020, health insurance programs do not cover the cost of doula services, but this has been widely advocated.
For example, if the support of a doula can potentially decrease the chances of a cesarean section, the cost of those services would be far lower than the cost of the operation.
Reproductive Endocrinologist
Reproductive endocrinology (RE) and infertility evolved as a subspecialty of obstetrics and gynecology to foster expertise related to the menstrual cycle, fertility, and the ability to maintain a pregnancy; RE also includes male fertility.
Reproductive endocrinologists manage complex problems with the reproductive organs, and are trained in procedures such as in vitro fertilization, gamete intrafallopian tube transfer, zygote intrafallopian transfer, and embryo transfer.
Women can be referred to an reproductive endocrinologist at any point recommended by an OB/GYN, to better evaluate fertility, reproductive disorders, hormonal imbalances, or recurrent pregnancy losses.
Medical Student
For pregnant women at a hospital or large university teaching hospital, they may encounter various medical students throughout their appointments or their labor/delivery.
Medical students need exposure to labor and delivery to gain experience but cannot be involved in a delivery or observe a cesarean section without the consent of the pregnant woman.
All physicians are required to inform a pregnant woman any time a student is either observing or participating, to include their level or education and training, to date. The woman will then decide whether to consent.
Medical students have different responsibilities and procedures they must follow depending on the university, hospital, and resident; students are not allowed to perform pelvic exams without a resident/HCP present. If a student is allowed to do a pelvic exam, and the woman consents, a resident or LDN will likely perform a second exam immediately afterward to check the student’s assessment.
Non-Obstetric Specialties
Pregnant woman may experience an illness, disease, symptom, or injury during pregnancy that requires an additional sub-specialist outside the field of obstetrics. It is not uncommon for women to see additional specialists during pregnancy.
The following are examples of specialties that deal with the diagnosis, treatment, and prevention of specific disorders:
Cardiologist: cardiovascular system (heart, blood pressure)
Gastroenterologist: gastrointestinal system (stomach, intestines, esophagus; also includes heartburn/acid reflux)
Orthopaedic Surgeon: musculoskeletal system (bones, joints, ligaments, tendons and muscles)
Endocrinologist: endocrine system (hormones)
Pulmonologist: respiratory system (upper and lower airways; lungs)
Nephrologist: kidneys
Neurologist: brain and nervous system
Otolaryngologist: Ear, nose, and throat
Ophthalmologist: Eyes/vision
Vascular Specialist/Surgeon: Blood vessels
Psychiatrist: mental health professional with a specific focus on medical management
Psychologist: behavioral health specialist (generally does not prescribe medication; state regulated)
Counselor: licensed professional offering counseling services to improve mental, social, and behavioral health (relationships, substance abuse, financial, rehabilitation)
Action
Women need to feel very comfortable with their HCPs during their pregnancy. It is recommended that women learn the different types, training, education, and responsibilities of each, and then determine the type of care and style that makes them the most comfortable.
Women should also read all about Appointments and current research regarding Birth Plans to accommodate their learning; this can also help them better understand different health care facilities and options available to them regarding their entire childbirth experience.
Partners/Support
It is important partners or other family members also attend regular prenatal appointments with the pregnant woman when possible. Partners can meet the HCPs caring for the woman/baby, ask their own questions and get familiar with the pregnancy and childbirth process.
All parties need to be comfortable and at ease with the HCPs the woman may encounter during pregnancy. It can get overwhelming at first, and women/their partners should always speak up, ask questions, ask for clarification, and make sure they leave every appointment understanding any situation or instruction necessary.
Resources
American College of Obstetricians and Gynecologists
To verify the credentials of an obstetrician, contact the American Board of Obstetrics and Gynecology.
The Association of Women's Health, Obstetric and Neonatal Nurses (AWHONN)
Maternal-Fetal Medicine Specialist (Find an MFM Specialist)
Association of Physician Assistants in Obstetrics & Gynecology
American Association of Nurse Practitioners
American Society of Registered Nurses
American College of Nurse-Midwives
North American Registry of Midwives
International Confederation of Midwives
Comparison of Certified Nurse-Midwives, Certified Midwives, Certified Professional Midwives (chart)
Accreditation Commission for Midwifery Education (ACME)
American Midwifery Certification Board (AMCB)
Find a Doula (Dona.org)