Cesarean Section Overview

Cesarean sections, in which the uterus is surgically cut open to deliver a baby, are commonly performed around the world as both planned and unplanned operations. Some women will know they will have a cesarean delivery early in their pregnancy, others may learn at or near delivery, and others may specifically choose a cesarean over a vaginal birth.
It is important that women are appropriately informed of the complete risks and benefits of undergoing a cesarean section before the end of pregnancy.
Even women planning a vaginal birth need to be aware of information regarding cesarean sections, the procedure, and the risks. Complications may arise near the end of term or during vaginal delivery, and all pregnant women should be prepared for the possibility a cesarean section may be needed.
If women learn ahead of time about the procedure, statistics, risks, possible complications, and what they can expect during recovery – even just in case – this can relieve significant anxiety, provide more time to ask questions, and women can feel more prepared and better informed if plans need to change quickly.
All women who may have questions regarding the right delivery method should have a risks and benefits discussion with their health care provider (HCP) that is individualized to their own pregnancy, as well as their physical, mental, and emotional health.
Background
A cesarean section (c-section) is a surgery in which the abdomen and uterus are cut to deliver a baby. Between 1997 and 2010, c-section was the most common major surgical procedure performed in the United States (U.S.).
Traditional types of c-section were either called elective (by choice) or emergency but are now more commonly referred to as “planned” or “unplanned".
An estimated 85% of c-sections are performed for four reasons: a prior c-section, “failure to progress”, fetal jeopardy, or abnormal fetal presentation (breech).
In 1985, the World Health Organization recommended that countries aim for a c-section rate of 10% to 15% of all births. However, c-section rates are increasing worldwide:
31.9% in the United States (2015)
20% to 25% in the United Kingdom (2011)
28% in Canada (2017)
30.9% in Australia (2007)
90% in private practice in Brazil (2015)
This image contains triggers for: Procedure, Real Delivery, Surgery
You control trigger warnings in your account settings.
Planned Cesarean
Physicians weigh numerous factors in determining whether a planned c-section may be most beneficial, to include maternal age, fertility treatment, obesity, diabetes, previous pregnancies, prior c-sections, and the overall health of the woman and baby:
Breech presentation: The American College of Obstetricians and Gynecologists (ACOG) issued a committee opinion on breech delivery stating that “patients with a persistent breech presentation at term in a singleton gestation should undergo a planned cesarean delivery".
Prior c-section: Women who had a prior c-section may be able to give birth vaginally. The decision depends on the type of incision used in the previous c-section, the number of prior c-sections, whether the woman has any conditions in which a vaginal delivery would be riskier, as well as other factors. However, it is estimated that most c-sections performed are repeat operations.
Other reasons for a planned c-section may include:
Multiple pregnancy: usually because at least one baby is in an abnormal position
Preterm birth
Small for gestational age
Mother to child transmission of viruses such as HIV, Hepatitis B, Hepatitis C, or Herpes
Conditions in the mother such as diabetes, high blood pressure, or preeclampsia
Maternal request (see section below)
Controversial reasons for a planned c-section include the potential for a “large” baby and postterm pregnancy.
About 1 in 10 women whose planned c-sections are scheduled for 39 weeks will go into labor first, meaning their membranes rupture or contractions start. Women are advised to call their HCP immediately if this occurs.
This image contains triggers for: Blood, Procedure, Real Delivery, Surgery
You control trigger warnings in your account settings.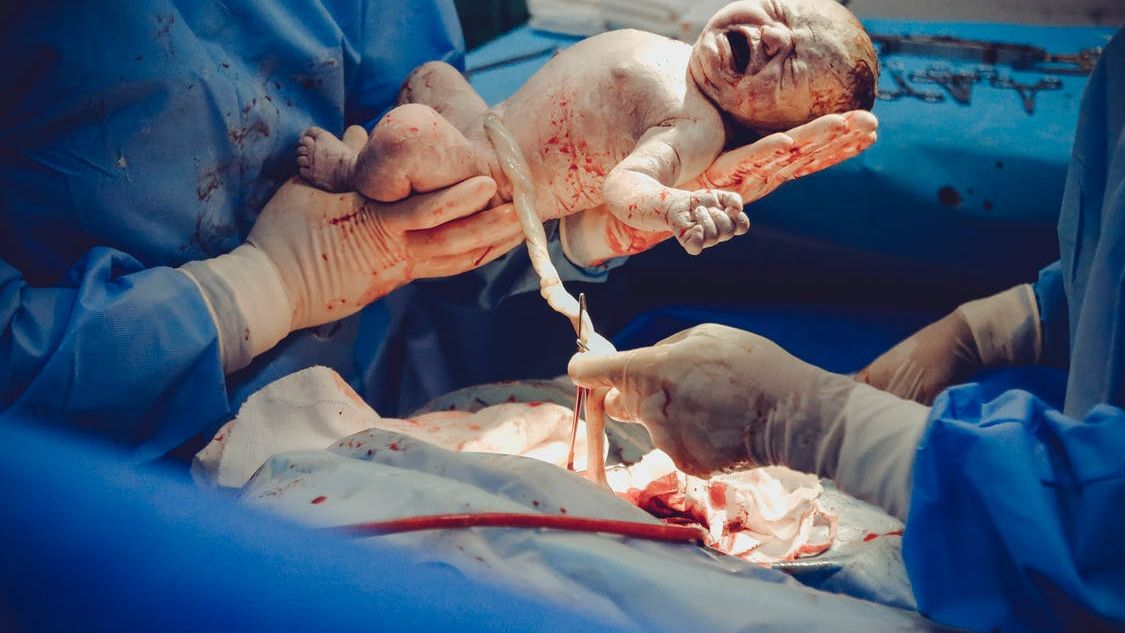
Maternal Request
A growing number of women are requesting delivery by “elective” c-section without a conventional medical reason, or “cesarean delivery upon maternal request”. These types of c-sections have doubled over the past decade, with up to 4% to 18% of all c-sections done at the mother’s request. Some country-specific rates are even higher.
There are many documented reasons a woman may specifically choose a c-section over a vaginal birth, even when there is no medical reason indicating she needs one.
Fear appears to be the top influential factor; more specifically, fear of complications, fear of childbirth, safety concerns, dysfunctional beliefs about childbirth, and/or previous traumatic birth(s).
It has been recommended that when a woman requests a c-section because she has a fear of childbirth, she should be offered counseling and educational support, which could lessen her both her fear and pain during labor and delivery.

However, it has been noted that c-section on maternal request should not be motivated by the unavailability of effective pain management, when there are numerous safe and effective options available.
Some women, based on cultural and/or social reasons, may also just prefer the convenience and control of being able to plan the precise timing and day of delivery.
Women may also choose a c-section based on incorrect or misleading information about risks, benefits, and complications of c-section versus vaginal delivery. When women are given correct information about risks and benefits, they may either reverse their decision or be more confident in selecting a c-section based on the overall health of their pregnancy (see below, Risks and Complications).
Several published reviews have attempted to determine a way to document the risks and benefits of specifically choosing a c-section. However, there is insufficient information from clinical studies to counsel women about which approach to the delivery – especially their first delivery – is clearly better.
There are no randomized controlled trials comparing planned c-section versus planned vaginal birth for non-medical reasons at term, and it would be difficult to design a study that would be ethical, and “will likely never be done".
Therefore, any woman who desires to have a c-section should have an individualized conversation with her HCP, regarding the risks and benefits of planned cesarean vs. planned vaginal delivery, tailored specifically for that woman's pregnancy, as well her overall physical, mental, and emotional well-being.
This image contains triggers for: Blood, Procedure, Real Delivery, Surgery
You control trigger warnings in your account settings.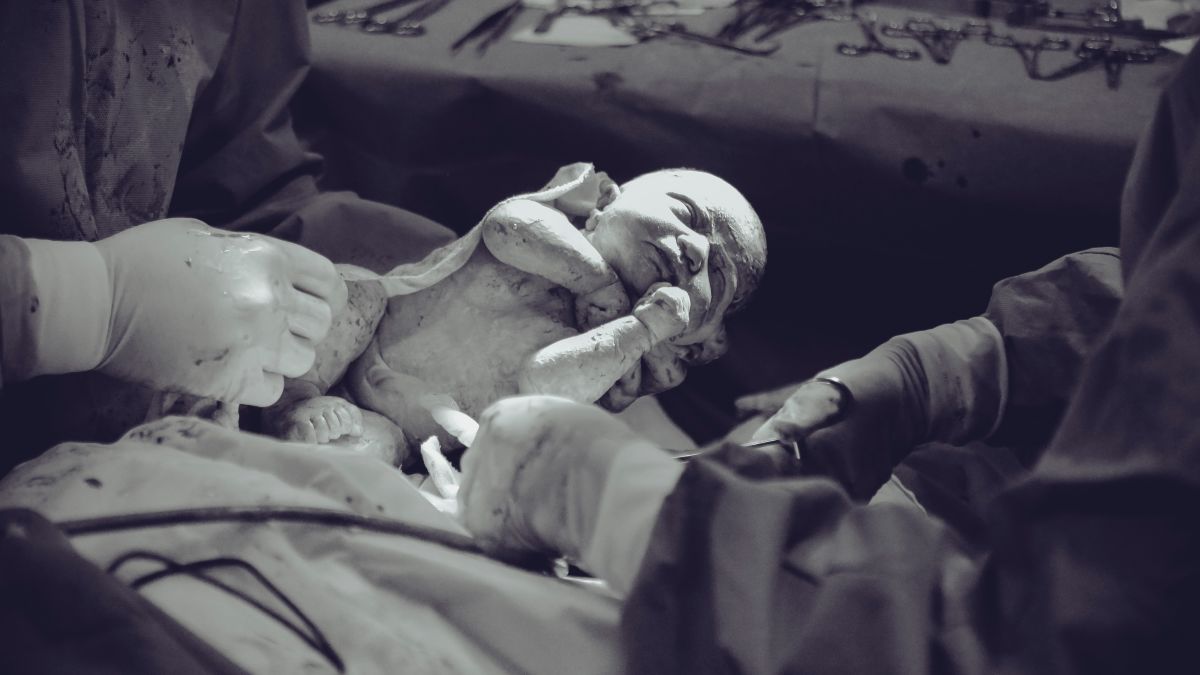
Maternal Request – Factors to Consider
HCPs will help a woman determine whether a planned c-section will be more beneficial or harmful to a specific woman and her baby compared with vaginal birth.
ACOG guidelines recommend that HCPs and mothers work together to assess how the risks and benefits of planned c-section apply specifically to each woman. ACOG supports the concept of a c-section on maternal request, given that the mother has been guided by high-quality informed consent.
There are some important factors women should consider in their decision to specifically choose a c-section without a medical reason.
C-section is generally not recommended for women who are planning more than one child because of the potential for placental complications. Risks of placenta previa, placenta accreta, uterine rupture, and hysterectomy increase with each cesarean delivery.
It is also not recommended for those seeking to avoid urinary problems, such as incontinence (leaking). Pregnancy itself can cause these urinary changes and symptoms, not just vaginal delivery, and c-section is not completely protective of these. Although c-sections are associated with a better short-term outlook for these symptoms, it likely has no effect on long-term changes, especially after additional pregnancies.
Newborn health (prior to full term): There is a significant risk of respiratory complications in infants born by elective c-section in early term gestation (37+0 to 38+6 weeks). This is one of the reasons HCPs will ask women to wait until at least 39 weeks.
When a woman desires a c-section on maternal request, the HCP will consider her specific risk factors, such as overall health, age, body mass index, gestational age, reproductive plans, and personal and cultural values.
If the HCP believes that performing a c-section would be detrimental to the overall health and welfare of the woman and her fetus, the HCP is ethically obliged to refrain from performing the surgery.
Although it is currently unknown if a c-section on request improves mental well-being in the mother, this potential benefit could outweigh the increased risk of c-section complications. This has led some researchers to ask the reverse question of whether more harm could be done if the mother’s request is not granted.
An HCP’s insistence on a vaginal delivery could induce additional stress on the mother and possibly increase the risk for anxiety and depression, both during and after pregnancy.
Both the ACOG and the United Kingdom’s National Institute for Health and Clinical Excellence (NICE) guidelines advocate that in this case, a woman’s decision should be respected, and she should be offered referral for a second opinion.
Unplanned Cesarean
Unplanned c-sections are surgical deliveries determined near the end of term or after labor has already started, or failed to start, and a vaginal birth was planned. Unplanned c-sections usually occur due to:
Failure of labor to progress
Fetal intolerance of labor
Abnormal fetal heart rate/distress
Abnormal position (determined either before or after labor has begun)
There is little evidence to guide HCPs about exactly when a c-section is necessary once labor has begun, and the decision lies mostly on the experience of the HCP.
Risks and Complications
Overall, c-section has higher surgical risks for current and subsequent pregnancies compared with vaginal delivery, but in general, these complications are considered rare in normal, healthy pregnancies.
The risks for bleeding and hemorrhage are debated; although the risk for severe bleeding from the placenta is lower in a c-section, abdominal surgery itself carries a high risk of bleeding problems. There is also a higher risk of blood clots after a c-section.
Anesthesia complications and the chance of infection are higher in c-section than vaginal delivery (but still low).
Less common risks include injury to the bladder, ureters (tubes that connect the kidneys to the bladder) and intestines.
Some women develop a weakness in the abdominal wall (hernia) following abdominal surgery, which may require another surgery.
A large nationwide study published in July 2021 found that the risk for a serious cardiovascular complication within 42 days after delivery was more than twice as high after cesarean section compared with vaginal delivery (but absolute risk was low). Cesarean section is a major abdominal surgery that can put stress on the cardiovascular system.
This image contains triggers for: Procedure, Real Delivery
You control trigger warnings in your account settings.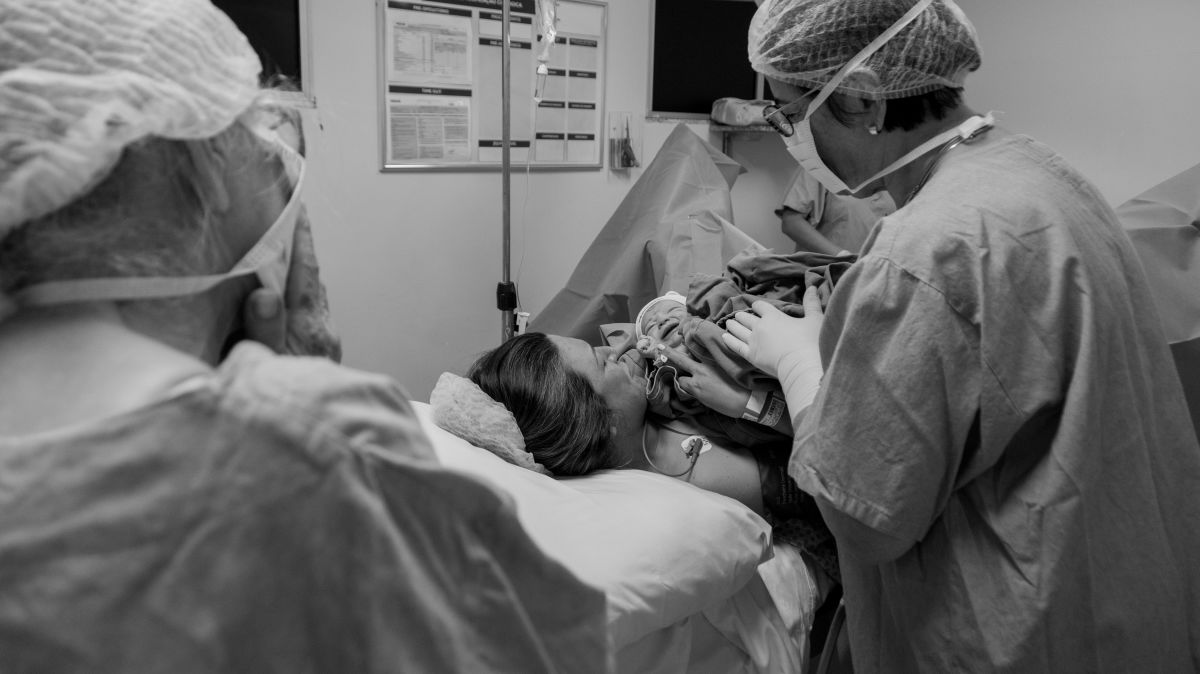
Other rare complications of c-section include:
Need for further surgery
Admission to intensive care unit
Trouble urinating or urinary tract infection
Delayed return of bowel function
Delayed wound healing
Abdominal discomfort
Emergency hysterectomy
Death (0.01 to 0.02%)
Complications increase with each repeated cesarean, but overall risk remains low.
Second stage c-section, which is a c-section performed after dilation and effacement is complete and vaginal delivery has been attempted, has a considerably higher potential for additional risks and complications, especially for a deeply engaged head.
These complications include bladder injury while opening the abdomen, difficulty in delivery of the head, broad ligament hematoma, tear of the lower uterine segment, accidental incision over the vagina, and pelvic organ prolapse.
Potential benefits over vaginal delivery include lower rates of perineal injury and short-term pelvic floor disorders, as c-section avoids stretching and tearing of the muscles and nerves that occurs as the baby's head comes through the pelvis.
However, as described above, pregnancy itself can cause pelvic floor changes and symptoms, not just vaginal delivery.

Postpartum pain is reported to be higher after c-section than vaginal birth and recovery time is longer.
A study looking at fatigue and quality of life found that women who had a vaginal birth generally recovered to their baseline by three weeks after delivery while women who had a planned cesarean took six weeks to recover; women with an unplanned c-section took even longer to recover.
In one study of c-section postpartum pain, pain was experienced by almost 80% of women eight weeks after delivery (compared with 50% of women with vaginal delivery) and was described as a “major problem” by 33%.
For the baby, c-section includes the possibility of fetal laceration (2%) and greater rates of initial respiratory difficulties, requiring oxygen.
Unborn infants have fluid in their lungs and labor contractions help move this fluid out of the lungs. Without contractions, babies may have difficulties breathing and may require intensive care or monitoring.
In 1916, Dr. Edward Cragin wrote “once a cesarean, always a cesarean”. Although an automatic c-section for a subsequent pregnancy is no longer the rule, women are more likely to have a c-section in a subsequent pregnancy, which further increases the risks above.
Procedure
Cesarean section is one of the most performed surgical procedures in the United States and around the world, and the procedure itself is done very similarly across all countries. Click here for a detailed description of the procedure.
Action
Women should refer all their questions regarding cesarean section, and the possibility of cesarean section, to their HCP.
Women planning a vaginal birth need to be aware of information regarding cesarean sections, the procedure, and the risks. Complications may arise near the end of term or during vaginal delivery, and all pregnant women should be prepared for the possibility a cesarean section may be needed.
Resources
Read about the history of cesarean section: A detailed article on the history of cesarean deliveries can be read on the website for the U.S. National Library of Medicine, History of Medicine.