Pregnancy Loss (Overview)

The widespread use of highly sensitive home pregnancy tests has allowed women to find out they are pregnant within 8 days of conception. While this extra time is a positive development in allowing women to prepare for a pregnancy much earlier, it has also revealed just how many pregnancies are lost in the first few weeks.
The prevalence of miscarriage is so high in humans, that scientists have called it "inefficient" and an absolute "paradox".
Although recognizing its high frequency does not make experiencing it any easier, this same research reveals that most couples who experience miscarriage go on to have healthy, full-term pregnancies in the future.
While researchers continue to study the potential causes of miscarriage and try to develop new treatments, couples should know they should not give up hope and they can ask for assistance from an HCP at any time.
Background
Clinically, there are several different "types" of miscarriage. Even though they all result in loss, understanding the distinctions between each may help some women understand better what is happening, why a test was positive before turning negative, why an early ultrasound exam was deemed "inconclusive", or why they are bleeding and what it might mean.
Further, this information may also help women recognize why it is very difficult for HCPs to determine if a pregnancy will continue.
Miscarriage is generally defined as the spontaneous (unplanned/natural) loss of a pregnancy prior to 20 weeks’ gestation. Other organizations define it as loss prior to 24 weeks, the time frame in which a fetus is usually viable outside the uterus.
There are several different terms associated with different types and stages of early pregnancy loss:
Threatened miscarriage: Bleeding is present, but the cervix is closed; it is completely possible the pregnancy will continue, and miscarriage does not occur.
It is estimated that 25% of women who present with threatened miscarriage will go on to miscarry – 75% of women will continue with a healthy pregnancy. Causes of bleeding in the first trimester are detailed here.
Missed miscarriage: An ultrasound reveals the embryo has passed, but the body has not yet started to resolve the loss.
Clinical miscarriage: Ultrasound examination or laboratory evidence has confirmed an intrauterine pregnancy existed, and the body has started the resolution process.
Incomplete miscarriage: Passage of some pregnancy‐related tissue, but with evidence of retained tissue (via ultrasound).
Complete miscarriage: a miscarriage that has fully resolved, and confirmed through negative pregnancy test (a complete miscarriage could take between 7 to 60 days to fully resolve).
Recurrent pregnancy loss (RPL): Most organizations define RPL as 3 or more consecutive losses prior to 20 or 22 weeks; however, the American Society for Reproductive Medicine defines it as 2 or more clinical pregnancy losses (documented by ultrasound or laboratory examination), but not necessarily consecutive. It is estimated that 1% to 2% of women experience RPL.
RPL is a very frustrating condition for both couples and their HCPs when a reason for consecutive losses cannot be determined – which is likely multifactorial. It is estimated however, that a cause for RPL can be identified 40% to 60% of the time. Fortunately, studies reveal that couples who do experience RPL still have a very good change of a future successful pregnancy.
Statistics
Statistics regarding miscarriage are only estimations at best, but do consistently indicate its frequency in all ages, races, and ethnicities. It is very difficult, if not impossible, to know true rates of miscarriage as well as the different types, as many women may never see an HCP from the time of a positive test to a complete miscarriage.
However, it is routinely estimated that only 30% of all conceptions result in a live birth.

As such, miscarriage remains a common outcome of pregnancy, affecting millions of women annually. A quarter of a million pregnancies are estimated to miscarry every year in the United Kingdom and up to 1 million pregnancies in the United States (although not all are recognized).
Miscarriage is also common in women who already have one or more children. This high rate of miscarriage has led to the description of human reproduction as “inefficient” and an evolutionary “paradox".
For women experiencing a miscarriage, or who have experienced one before, the probability a future pregnancy will be successful is very high.
In one study, women who had experienced up to five miscarriages had an average of three children, and those with more than six miscarriages had an average of four children.
Two or three consecutive pregnancy losses is less common, but even women with recurrent losses have a high chance of a successful future pregnancy.
Early Pregnancy Loss – General
Very early pregnancy loss can present as a positive home pregnancy test but:
A woman tests again a few days later and the test is negative (biochemical)
Further testing is positive, but an ultrasound shows a large empty gestational sac (anembryonic) when an embryo should be present
Further testing is positive, but an ultrasound reveals a pregnancy that may not be in the uterus (ectopic pregnancy)
Further testing is positive, but an early ultrasound reveals pregnancy-related structures that are too small/missing for gestational age (intrauterine pregnancy of uncertain viability)
Further testing is positive, however, a woman begins heavy bleeding, similar to her menstrual period, and subsequent testing is negative
In the last scenario, in which an HCP cannot determine whether the pregnancy is viable, an additional ultrasound is normally scheduled for a week or two later.
A woman may also experience a missed miscarriage, in which an HCP determines via ultrasound a miscarriage has occurred, but the women has not yet experienced any bleeding (a pregnancy test may still be positive).
Anembryonic Pregnancy (Blighted Ovum)
An anembryonic pregnancy (formally called a blighted ovum) occurs when a fertilized egg implants but does not develop, and is then reabsorbed by the body, leaving an empty gestational sac. A pregnancy test can be positive because the secretion of HCG occurs as implantation is attempted/completed.
This type of pregnancy loss was first recognized in the 1970s as ultrasounds became more popular and were used earlier, which allowed for the visualization of different types of early loss for the first time.
Diagnosis of an anembryonic pregnancy is made when an ultrasound shows a gestational sac with no embryo or yolk sac, as long as the empty gestational sac is at least 18 to 25 mm (greater than 2 cm). This large range exists due to different organizational guidelines for diagnosis.
If the gestational sac is smaller than 18 mm, it is possible gestational age is wrong and it is too early to see any additional structures. HCPs will usually wait until the larger end of this range (25 mm) before confirming a loss.
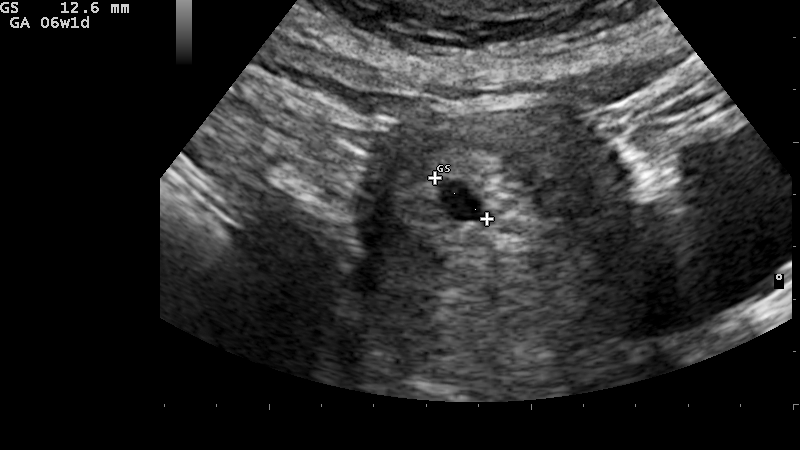
With anembryonic pregnancies, common symptoms of early pregnancy are usually present, such as breast tenderness, nausea, abdominal cramping, and potentially spotting and/or heavier bleeding.
Biochemical Pregnancy
A biochemical pregnancy occurs when a pregnancy test is positive, but the pregnancy is either not confirmed on ultrasound (no signs of pregnancy can be observed) or an additional pregnancy test taken a day to several days later is negative.
This type of loss is called a biochemical pregnancy because it was only confirmed through the presence of HCG. A biochemical pregnancy is considered the earliest type of loss that can be recognized; fertilization was successful, implantation was attempted, but no structures developed. This loss usually resolves quickly, and in some cases, only delays menstruation by a few days.
It is estimated that biochemical pregnancies are very, very common. One study documented 442 biochemical pregnancies in only 681 cycles. Biochemical pregnancies are also common following in vitro fertilization (IVF).
The probability of a future successful pregnancy in women who experience biochemical loss is excellent, and most women will go on to experience a full-term pregnancy. Further, biochemical loss is not associated with the failure of future IVF cycles.
Ectopic Pregnancy
Ectopic pregnancy occurs when a fertilized egg implants and grows outside the main cavity of the uterus, usually in a Fallopian tube. A fertilized egg can also implant in the cervix, ovary, abdominal cavity, prior cesarean scar, or where the uterus and Fallopian tubes meet, but these are very rare.
Ectopic pregnancy is considered a gynecological emergency because if left undiagnosed and untreated, the developing embryo can cause the Fallopian tube to rupture, which is life-threatening and requires surgery.
Because some of the same symptoms of ectopic pregnancy occur in a normal intrauterine pregnancy, women need to call their HCP anytime in early pregnancy if they are experiencing any pain or bleeding, as ectopic pregnancy needs to be ruled out (read more).
Molar Pregnancy
Gestational trophoblast disease (GTD) is a group and range of very rare conditions of pregnancy loss that cause tumors to grow in the uterus (also known as gestational trophoblastic neoplasia). These tumors grow from the trophoblast cells that develop into the placenta.
The most common form of GTD is hydatidiform mole, also known as molar pregnancy. These are abnormally fertilized eggs that result in loss; additionally, some molar pregnancies have the potential to become malignant (read more).
Action
Women who experience bleeding in early pregnancy should call their HCP. Even though bleeding does not always mean a miscarriage will occur, it is important to rule out the possibility of an ectopic or molar pregnancy, especially if pain is also present.
Miscarriage, when it does occur, can be devastating, especially for couples who have experienced multiple losses. Women who are trying to conceive need to keep in mind, that even though it may seem everyone around them is conceiving, miscarriage is often hidden, and they are certainly not alone.
Additionally, they should not give up hope; most women who experience even more than one miscarriage go on to have healthy pregnancies in the future.
The overall causes of miscarriage are considered multi-factorial – indicating it is likely that more than one factor acted simultaneously that resulted in loss – most of which are completely out of a couple's control. Fortunately, some causes can be identified and treated, which could greatly increase the changes of a successful pregnancy, faster (read Causes of Miscarriage).
For women who have been diagnosed with a missed, incomplete, or inevitable miscarriage, they have several options for moving forward (read Management of Miscarriage).
Women grieve and handle loss differently. Some women can move forward rather quickly, while others need more physical, emotional, and/or mental health support. Women should lean on each other, share their experience below, and ask their HCPs for resources, which includes support groups and opportunities for counseling.
Resources
Early Pregnancy Loss Practice Bulletin (American College of Obstetricians and Gynecologists)
RESOLVE.org (Support)