Skin

Regarding noticeable physical signs and symptoms, skin changes may affect more pregnant women than any other organ system. It is estimated that 90% to 100% of all pregnant women will experience at least one sign or symptom related to changes of and within the skin.
These can include stretch marks, dry skin, pigmentation, itching, skin tags, acne, and eczema, as well as specific conditions during pregnancy that can manifest through the skin (due to liver and immune system changes).
Some symptoms and conditions are easily treated, while others can cause complications if left untreated. Women should read the below to better understand their skin during pregnancy, as well as signs/symptoms to be aware of and when to call their health care provider (HCP).
Background
During pregnancy, hormones and changes to the immune system and blood vessels influence the skin in various ways. Since women respond differently across all three of these major systems (i.e. genetics), women will experience different changes in their skin and to different degrees of severity.
It is estimated that most – if not all pregnant women – will notice at least one skin change during pregnancy.
Skin changes are either pregnancy specific, existed prior but get worse during pregnancy, or conditions that are new and unrelated to pregnancy, but occur while a woman is pregnant.

Researchers and clinicians have tried to categorize these skin changes; these categories can be confusing as some of the same conditions have different names. However, four categories are generally accepted:
Atopic Eruption of Pregnancy (which is a combination of eczema, itching, and pruritic folliculitis of pregnancy)
Polymorphic Eruption of Pregnancy (also known as Pruritic Urticarial Papules and Plaques of Pregnancy or PUPPP)
Pemphigoid Gestationis
There are also uncategorized general changes to the skin that include pigmentation, stretch marks, extreme dryness, varicose veins, itching, acne, and skin tags.
Most skin conditions during pregnancy are minor and either resolve or fade postpartum. Other conditions may require specific treatments or require monitoring. Any pregnant woman who notices something new or possibly abnormal regarding her skin should talk to her HCP.
Pigmentation
Changes in skin pigmentation (melasma or chloasma) during pregnancy are experienced by up to 90% of pregnant women and is considered one of the earliest signs of pregnancy.
It starts from the first trimester and occurs in areas that are already pigmented, such as the nipples, areola, genital areas, around the eyes and eyelids, and the midline of the abdomen, known as the linea nigra.
The linea nigra is a vertical line that typically runs from the pubic bone to the belly button, but can run all the way up to the chest.
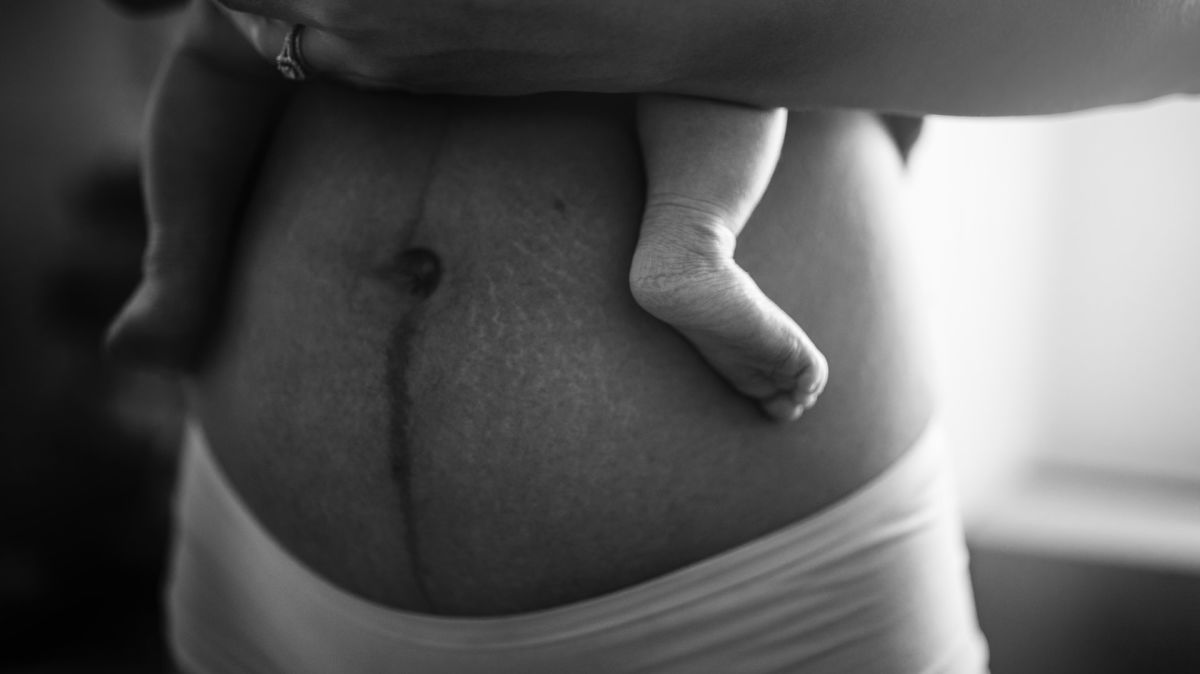
This line already exists in both men and women, but simply gets darker in females during pregnancy, indicating that the likelihood of having a linea nigra may depend on a woman's level of sex hormones.
It is theorized that estrogen, progesterone, and components of the placenta cause an increase in melanogenesis – the process that produces melanin; melanin is a type of dark pigment in the skin (sunlight also causes melanogenesis, resulting in a "tan").
Pigmentation usually fades after delivery, but may not disappear completely. It could also take months or years to fully fade.
Pregnant women may be able to prevent some pigmentation changes, or at least prevent them from getting worse/darker by avoiding excessive sunlight and using sunscreen.
Stretch Marks
Stretch marks are a well-known “side effect” of pregnancy. Research indicates that 50% to 90% of women will notice at least one stretch mark related to pregnancy that fades in the postpartum period.
Stretch marks are indented streaks in the skin that appear on the abdomen, breasts, hips, buttocks, and thighs due to rapid stretching. If growth occurs faster than the skin and its ability to stretch, it "tears". Stretch marks can vary in color from pink, red, blue, purple, or silver depending on the body part and age of the mark.
There are many theories as to why some women get stretch marks and others do not. However, research is very inconsistent, which makes recommendations regarding the prevention and treatment of stretch marks frustrating.
Overall, it appears that genetics likely play the biggest role in whether a woman develops stretch marks, which could also determine the level of relaxin a woman produces.
One study indicated that women who are more likely to experience stretch marks may have lower levels of relaxin in their blood, indicating the skin in these women may be less elastic.
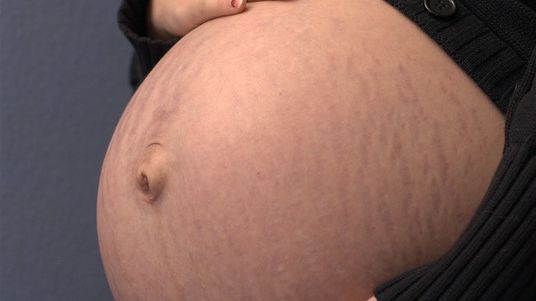
Weight gain is also commonly cited, based mostly on this being the most common causal factor in non-pregnant individuals with stretch marks. However, women can get stretch marks during pregnancy even with minimal weight gain. Additionally, although stretch marks usually develop in a first pregnancy, they can also occur for the first time in a subsequent pregnancy.
Due to a lack of knowledge regarding the formation of stretch marks during pregnancy, there is very little data regarding the most optimal treatment or prevention technique. Additionally, there is no high-level evidence indicating any topical cream or product can prevent, treat, or fade stretch marks.
More than 75% of pregnant women will use some type of cream or oil, but almost the same number of pregnant women will still develop stretch marks. Even when a product indicates it is clinically proven, those trials may be few, limited, or unpublished.
Some creams claim to lessen the appearance of stretch marks, but in time, stretch marks also fade on their own, so it can be difficult to determine if the cream or oil made a difference.
Cocoa butter and oil-based creams are not effective for preventing stretch marks; however, stretch marks themselves can be incredibly itchy, and these creams may provide temporary relief and help women avoid scratching, or scratching too hard.
A review of several studies found that utilizing creams or oils while gently massaging the skin (fingertips) may help to prevent stretch marks in pregnancy. However, information regarding this technique is very limited and preliminary. Further, the most optimal length of time to massage, how to massage, and whether to use a cream or oil is not known/was not indicated.
Postpartum non-topical treatments may include laser therapy, light therapy, acid peel treatments, collagen injection, laser lipolysis, radiofrequency techniques and microdermabrasion.
Acne
Exactly how pregnancy affects acne is not well understood, but hormones appear to be the primary factor. While some women experience no change or even improvements in their skin during pregnancy, a substantial number of women will experience a worsening of acne. Women have treatment options during pregnancy, and some over-the-counter products currently have positive safety profiles (read Acne during Pregnancy).
Note: Any woman currently taking an oral or topical retinoid medication for acne prior to pregnancy, and are currently pregnant, should call her HCP immediately who will very likely advise the woman to stop taking that medication or using that product (read Acne).

Psoriasis
Psoriasis is a chronic inflammatory disease that causes red, scaly, itchy and/or painful patches of the skin.
Despite the large population of women who have psoriasis and get pregnant, there is very limited information on the condition during pregnancy.
Because most of pregnancy can be considered an anti-inflammatory state, in general, women with inflammatory conditions during pregnancy, such as psoriasis, tend to get better. It appears that psoriasis may improve in about 50% to 60% of women; however, it remains “unpredictable” in the remaining 40% to 50%.
A study published in December 2021 included a cohort of 3737 women with psoriasis, among a total of 13,792,544 pregnancy admissions in US hospitals between the years 1999 and 2015. The study revealed that psoriasis during pregnancy was associated with a higher risk of preeclampsia, gestational diabetes, and several other potential complications. The authors concluded, "It would be prudent for these women to be followed closely during pregnancy by their obstetrical caregiver and dermatologist."
Since some women still experience moderate to severe psoriasis during pregnancy, moisturizers and topical steroids or ultraviolet B phototherapy are considered the first-line treatment options for these women.
However, some HCPs may advocate stopping certain medications during pregnancy, especially if psoriasis is mild, and the fetus appears to be unaffected. Women with psoriasis during pregnancy need to discuss their symptoms with their HCP, and determine the risks and benefits of medication use specific to their own pregnancy.
Itching
Mild itching is common in pregnancy especially in locations where the skin has stretched and the skin is incredibly dry. An increase in blood supply also brings more blood closer to the skin, increases heat, and can contribute to itching.
The most affected sites of itching include the abdomen, breasts, and scalp, and usually begins in the second or third trimester.

Itching can be extremely frustrating for pregnant women. It can cause significant irritation, restlessness, trouble sleeping, and some women may even scratch too hard, which irritates the skin further or causes bleeding.
Creams, such as aqueous cream with menthol, and other moisturizers are considered safe to use in pregnancy and can provide some (temporary) relief from itching.
Although itching is very common and usually completely harmless, there are skin conditions during pregnancy that begin with itching (usually severe/extreme itching). Women with intense itching during pregnancy, or those who develop a rash, need to call their HCP so these conditions can be ruled out.
Polymorphic Eruptions of Pregnancy
Polymorphic Eruptions of Pregnancy (PEP), or Pruritic Urticarial Papules and Plaques of Pregnancy (PUPPP), is the most common skin condition that occurs in pregnant women.
PEP presents as a rash similar to hives that tends to start in the third trimester, in or near stretch marks in the abdomen, then spreads to the rest of abdomen, breasts, and arms and legs. PEP usually does not affect the face (but can). These lesions may also have a halo-looking effect in some women. Itching can be unbearable and HCPs can help women manage this condition (read Polymorphic Eruptions of Pregnancy).
Intrahepatic Cholestasis of Pregnancy
Extreme, intense itching that seems to have no relief should be assessed by an HCP and could be a condition known as Intrahepatic Cholestasis of Pregnancy (ICP). ICP is a potentially serious liver disorder also known as obstetric cholestasis, cholestasis of pregnancy, jaundice of pregnancy or pruritus/prurigo gravidarum (read Intrahepatic Cholestasis of Pregnancy).
Gestational Pemphigoid
Gestational pemphigoid is an autoimmune blistering disease known to be associated almost exclusively with pregnancy. It can start out very similarly to PEP, but spreads out further and progressively gets worse.
Large, tense blisters can form after a few weeks around the edge of the rash or in new areas of the skin. A noticeable “flare-up” at the time of delivery is also common.
Gestational pemphigoid is very rare, affecting between 1 in 1,700 and 1 in 50,000 pregnancies. It can also occur with gestational trophoblastic diseases (molar pregnancies). Diagnosis is made with a skin biopsy.
Topical and oral corticosteroids and antihistamines are recommended, as the condition usually resolves partially after delivery and completely within a few weeks or months.
Gestational pemphigoid recurs following menstruation, intake of oral contraceptive pills, and/or during subsequent pregnancies. A risks and benefits discussion of method of birth control after delivery with an HCP is recommended.
The condition is related to other autoimmune diseases, especially Graves' disease. Therefore it is also recommended that thyroid function tests are performed in women with gestational pemphigoid to rule out/prevent other associated problems.
Examples: Images 1 through 6 (DermNetNZ.org)
Action
Itching/rashes: Women need to tell their HCP about any itching or rashes during pregnancy to determine if these symptoms are indicative of any other condition described above that may require additional monitoring or treatment.
Psoriasis: Women with psoriasis during pregnancy need to discuss their symptoms with their HCP, and determine the risks and benefits of medication use specific to their own pregnancy.
Stretch marks: While various creams and oils claim to prevent or fade stretch marks, there is a lack of high-quality evidence to back up these claims. However, moisturizers may be able to provide temporary relief from itching and dry skin.
Acne: Any woman currently taking an oral or topical retinoid medication for acne prior to pregnancy, and are currently pregnant, need to call their HCP immediately who will very likely advise the woman to stop taking it (read Acne).
Partners/Support
Partners/Support can help women with skin related changes during pregnancy by:
Helping her apply cream/lotion
Keeping her mind off any itching whenever possible and reminding her to avoid scratching too hard
Offer to change bed sheets if certain fabrics increase the sensation of itching
Making her feel less anxious or frustrated about any stretch marks, varicose veins, acne, or pigmentation changes by providing positive emotional support
Gaps
Are butter-based or oil-based creams better for itch relief?
Resources
Skin Conditions during Pregnancy (American College of Obstetricians and Gynecologists)
Common Skin Conditions During Pregnancy *includes photographs (American Family Physician)