Influenza

October 14, 2022: According to the U.S. Centers for Disease Control and Prevention, early increases in seasonal influenza activity have been reported in most of the United States, with the southeast and south-central areas of the country reporting the highest levels of activity. This activity is higher than this time last year. The most frequently reported viruses this week were influenza A (H3N2). There is currently no pregnancy-specific data yet for this current season (CDC FluView Tracker).
Influenza ("flu") is a common seasonal respiratory infection that can be more severe in vulnerable populations. It is often indicated that pregnant women are more susceptible to influenza infection, or may experience more severe illness.
However, severity of influenza infection – and its prognosis during pregnancy on both mother and baby – appears to depend upon: stage of pregnancy, underlying illnesses, vaccination status, the overall health of the pregnancy, and at which point the woman sees a health care provider (HCP) or receives medical care for the infection.
It is recommended all pregnant women get vaccinated. This current season is expected to be potentially severe and is running concurrently with the ongoing COVID-19 pandemic. It is possible to contract both viruses at the same time.
Not all pregnant women who contract influenza will have serious illness, but there is currently no way to determine which women may experience a more severe course of the disease. Therefore, the earlier a woman is seen, tested, diagnosed, and treated, the better the prognosis.
Current research indicates the best way pregnant women can protect themselves and their babies is to practice good hygiene, get vaccinated, and call their HCPs immediately when they have a fever or believe they may have the flu.
*If you are experiencing trouble breathing or extreme shortness of breath, seek emergency medical care immediately or dial 911*
Most Recent Updates:
October through May is considered influenza season in the United States. See more information on the current season below under "Ongoing Now".
October 14, 2022: Early increases in seasonal influenza activity have been reported in most of the United States, with the southeast and south-central areas of the country reporting the highest levels of activity (CDC FluView Tracker). Highest activity is reported in Georgia, New York City, South Carolina, Tennessee, Texas, Virginia, and Washington D.C.
Read Vaccines for more detailed information specific to the influenza vaccine during pregnancy.

Background
Influenza, also known as "the flu", is a respiratory disease caused by influenza viruses. It is estimated that three to five million cases of severe influenza (millions more mild cases) occur annually worldwide, resulting in 250,000 to 650,000 deaths.
Pregnancy is considered a risk factor for developing severe influenza infection, which has been reported by different countries all over the world; pregnancy may also be a stronger risk factor than obesity, diabetes, and cardiovascular disease.
There are four types of influenza viruses:
Influenza A (seasonal epidemic; responsible for all three prior pandemics)
Influenza B (seasonal epidemic)
Influenza C (rare, mild infections)
Influenza D (does not affect humans)
Influenza is further categorized by two surface proteins: hemagglutinin (H) and neuraminidase (N), which lead to the familiar naming conventions such as H1N1 and H3N2; each of these subtypes is a different strain (there are over 100 different combinations).
Seasonal Influenza: occurs annually and usually peaks between December and February; manageable impact on society, although some schools may temporarily close and workers may take more sick leave.
In a single flu season, it is estimated that 20% of the United States (U.S.) population contracts the illness, with the number increasing to 50% during pandemics. It is also estimated that 10% of pregnant women will have laboratory-confirmed influenza, with many more likely contracting the infection without official diagnosis.
Pandemic Influenza: global outbreak of a new influenza virus in which there is no vaccine or treatment (currently occurring with COVID-19); may cause major impact to the general public, such as travel restrictions and school or business closings; also includes severe impact on domestic and world economies; there have been four influenza pandemics in the last 105 years, all of which were documented to be more severe in pregnant women.
Historical Pandemics and Pregnancy
Most of what has been learned regarding pregnancy and influenza has come from data collected during the influenza pandemics of 1918, 1957, 1968, and 2009.
Pregnant women were at high risk of complications such as viral pneumonia, pulmonary edema, and maternal and fetal death; this is consistent with seasonal influenza, which also sees a disproportionate increase in hospitalizations and severe illness in pregnant women.
The 1918 “Spanish flu” killed 675,000 persons in the U.S., with an overall case fatality rate of 1% to 2%; however, pregnant women had a fatality rate of 27%; half of these cases included pneumonia. Further, during the 1957 pandemic, of all the reproductive-aged women who died, 50% were pregnant.
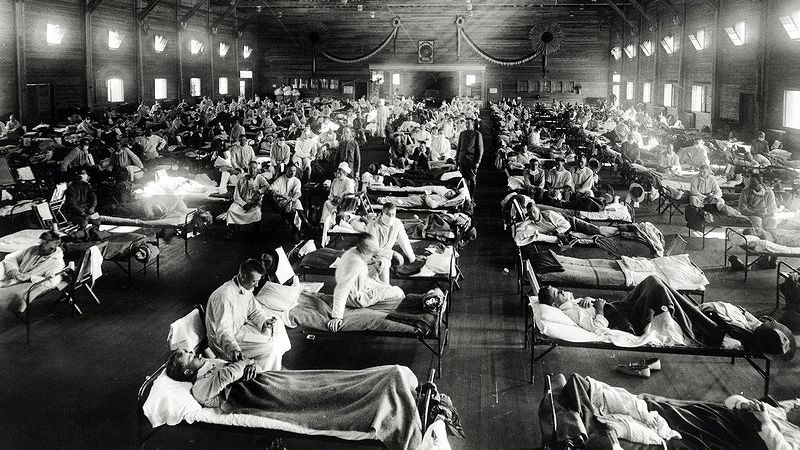
During the 2009 novel H1N1 pandemic, pregnant women accounted for up to 6.3% of influenza‐associated hospitalizations, 5.9% of Intensive Care Unit (ICU) admissions, and 5.7% of deaths, even though pregnant women make up only about 1% of the U.S. population at any given point. Even after the pandemic was declared over, several regions were still reporting high infection rates in pregnant women.
During this pandemic, the U.S. Centers for Disease Control and Prevention (CDC) recommended for the first time that antiviral drugs be given to all pregnant women with influenza as well as those considered at high-risk of influenza exposure.
Of all pregnancy-related deaths (for any reason) that occurred during the 2009–2010 pandemic season, 12% were attributed to influenza.
More specifically, the 2009 pandemic illustrated a severity difference by trimester; the third trimester was more evidently severe than earlier in pregnancy (see Trimester Severity below).
Symptoms
Flu symptoms in pregnant women are similar to the general population and include fever and cough (most common), sore throat, runny or stuffy nose, body aches, headache, chills, and/or fatigue. Some people may also have vomiting and diarrhea (usually children).
Maternal Complications and Risk Factors
Due to changes within women's respiratory, immune, and cardiovacular systems, pregnant women may experience more severe influenza infection that can manifest as miscarriage (debated), fetal death, eclampsia, pneumonia, or heart failure. Some of these complications have been associated with an increase in emergency cesarean section deliveries due to the mother’s worsening condition.
A study published in May 2021 indicated that of 15.9 million emergency department encounters for influenza, 4% occurred among pregnant women (n=636,000). Pregnant women with influenza were nearly three times as likely to be admitted as nonpregnant women. Once admitted, these women were at 72% higher risk of ICU-level interventions.
Pneumonia is likely a major factor regarding complication risk. Women hospitalized during the 2009 pandemic had a significantly increased risk of preterm delivery if they developed secondary pneumonia compared with those who did not develop pneumonia (71% vs 27%).

However, the incidence of complications and prognosis on pregnancy outcome appears to be related to the severity of the mother’s infection. For example, while pregnant women do have a much higher risk of serious complications, many others recover normally as outpatients, with no major complications.
Further, while pregnancy itself is a risk factor, underlying conditions may also play a role. Diabetes, asthma, obesity, and cardiac issues are also associated with increased severity of influenza infection; however, the data on influenza infection of specific pregnant women who are obese or have diabetes, asthma, or cardiac concerns is not known.
Trimester Severity
Susceptibility: A study published in July 2021 assessing influenza infection by trimester of pregnancy in more than 18,000 women determined that influenza infection was common in all three trimesters, indicating that pregnant women are equally susceptible to infection throughout pregnancy.
Severity: However, while influenza infection can be serious during any trimester, it does appear to be more severe in the second and (mostly) third trimesters.
Recent research on how the immune system changes during pregnancy may offer an explanation:
Previously, the leading hypothesis was that the mother’s immune system must be significantly suppressed in order to allow pregnancy to occur. The latest research points to a reversal in this hypothesis, indicating the immune system is actually quite active, and just modulated, not suppressed.
Early pregnancy is therefore considered a pro-inflammatory state (which allows for implantation and rapid fetal growth), followed by a significant amount of gestation at an anti-inflammatory state (or “tightly controlled inflammation”), which then returns to a pro-inflammatory state again near term to initiate labor.

Because most of pregnancy can be considered an anti-inflammatory state, in general, women with inflammatory conditions during pregnancy (multiple sclerosis, psoriasis, rheumatoid arthritis) get better during pregnancy, and women who contract viral infections requiring an inflammatory response tend to get more severe infections (influenza, STDs).
For example, the anti-inflammatory state most of pregnancy prevents or slows down an inflammatory response to viruses such as influenza, but the inflammatory response is necessary to combat and prevent it from spreading quickly through the body.
In other words: if a disease creates inflammation, that disease or condition tends to improve during pregnancy, as pregnancy mutes that inflammation. If a disease is “treated” within the body with an inflammatory response, this response is therefore also muted in pregnancy, and the disease is then made more severe.
However, when a pregnant woman is in a pro-inflammatory state, such as early pregnancy or at term, an unusually strong hyperinflammatory reaction ("cytokine storm") can occur.
This response could be the theoretical cause of why influenza sometimes leads to severe lung inflammation and preterm birth during pregnancy. In this scenario, treatment may need to be based on reducing this inflammation, not just stopping the virus. This is some of the same research being conducted regarding COVID-19.
A September 2020 study added weight to the above. The [animal] study suggested the virus does not stay in the lungs but spreads throughout the mother's body through the blood vessels and into the circulatory system, triggering a damaging "hyperactive" immune response (as described above). The study authors noted this goes against the "suppressed" immune system theory, and described a "heightened" response.
Additional factors that are present in late pregnancy may also play a role:
Functional Residual Volume (FRC) is the amount of air left in the lungs after a normal exhalation; this extra air is essential, as it helps keep the small airways open. By the third trimester, FRC decreases by 20% to 30%. A lower FRC can lead to potential alveolar collapse, making women more susceptible to respiratory compromise during an infection.

Fetal Complications
There are several factors researchers consider when attempting to analyze influenza’s effect on the fetus:
First: Can influenza be directly transmitted to the fetus?
Second: If it affects the fetus, is it because the infection crossed the placenta or due to another mechanism?
Third: If it does not transmit to the fetus, how does the mother’s illness cause fetal complications? What aspects of the mother’s deteriorating health affect the fetus’ health?
Vertical transmission of influenza virus (passage from mother to baby during pregnancy) is possible but is considered quite rare. Note: Antibodies from influenza vaccination do transfer; anti-viral medication may transfer.
Although there is at least one fatal case reported in which influenza was detected in fetal heart tissue, direct infection from mother to fetus is considered very rare; infection of the placenta is seen slightly more often but is also uncommon (but studies are limited).
Influenza has been identified in the placenta and amniotic fluid in both fatal and non-fatal cases. [Maternal and fetal blood never directly mix – all blood, oxygen, and nutrient exchange is conducted through the placenta.] In cases in which influenza was detected in the placenta/amniotic fluid, no significant abnormalities in the fetuses were reported.
However, when the placenta is affected, influenza appears to result in a breakdown of the placental architecture, likely due to inflammation. Compromise of placental structure and function may lead to reduced oxygen and nutritional supply as well as a buildup of waste in the fetus (since the placenta cannot filter it out), which could result in harmful effects to the fetus.
No attempts have been made to determine whether the virus can cross the placenta during the first trimester, and experiments trying to do so in mice have not been successful; this may be another reason why the third trimester is associated with worse outcomes, but more research is necessary.
Although the placenta and amniotic fluid can contain the virus, this is still considered somewhat rare (described above). However, the mother’s uterine lining (decidua) may be much more vulnerable.
Studies suggest that influenza can spread from the mother’s blood stream to the decidua to replicate within the tissue and then infect the fetal membranes, which would lead to preterm birth.
Regardless of whether/when placental transfer can occur, there is strong evidence linking influenza to fetal complications. Therefore, it is possible the mother’s infection leads to other complications within her body that can directly affect the fetus, rather than the virus itself (i.e. fever, general inflammation, or hormonal imbalance).
Influenza infection during pregnancy has been associated with small-for-gestational age infants, lower birth weight, premature rupture of membranes, preterm delivery, and fetal death. These outcomes very likely heavily depend on severity of the infection, as most of these outcomes were seen in women who were hospitalized.
Fever: Maternal hyperthermia (heat exposure) is considered a human teratogen, and fever is often considered a potential cause of complications during pregnancy, depending on numerous factors. Read more.
General inflammation: As stated above, a super inflammatory reaction can occur in the body from influenza infection. That study’s author opined that during the third trimester, the pregnant body is getting ready to switch back to pro-inflammatory, which is needed for labor and delivery. Infection at this time could lead to an overlap of this process, leading to severe inflammation, ultimately resulting in preterm birth.
Hormone response: Influenza infection may reverse the hormonal environment required to establish and maintain a healthy pregnancy, which could lead to a potential drop in progesterone too early, leading to preterm birth.
After the pandemic of 1918, an obstetrician found that the number of neonates with birth defects increased significantly, and almost all these women had had influenza. Fortunately, current research has not shown a strong link to birth defects, likely due to increased screening, medical care, and vaccinations.

Diagnosis and Treatment
Pregnant women are advised to call their HCP as soon as they believe they may have influenza.
Influenza can be diagnosed through nasal swab which provides rapid diagnosis; however, laboratory confirmation is usually necessary. It is recommended that women get officially screened for influenza as many respiratory illnesses mimic the flu. Based on a lack of data, it is also important that pregnant women not take antiviral medication if diagnosis has not been confirmed.
If fever or severe symptoms are present, however, pregnant women need to have a risks and benefits discussion of treating the fever with anti-fever medications, such as acetaminophen, which is usually recommended, especially for high fevers (read Acetaminophen).
Antiviral treatment works best when given within the first 48 hours from the onset of symptoms. Data comparing the outcomes of pregnant women who received early treatment, compared to those treated at four days or later illustrates the importance of early diagnosis and treatment.
Data on the use and safety of antiviral drugs in the treatment of pregnant women with influenza from randomized controlled trials are lacking, but the information that is available is reassuring.
Oral oseltamivir is currently the preferred treatment for pregnant women because it has the most studies available to suggest that it is safe and beneficial; zanamivir may also be used; however, optimal dosing in pregnant women is not known.

Vaccination
Influenza vaccination of pregnant women is considered the best option to reduce risk of infection and its related complications. While ideally it’s recommended to get vaccinated by the end of October, it’s important to know that vaccination after October can still provide protection during the peak of flu season.
Pregnant women can receive a flu vaccine during any trimester. The flu vaccine and the COVID-19 vaccine can be given at the same time.
More than 40 years of research, data, and hundreds of thousands of vaccinations have demonstrated the safety and effectiveness of the influenza vaccine during pregnancy – for both pregnant women and their newborns (read Vaccines for more detailed information specific to the influenza vaccine during pregnancy).
Note: It takes approximately two weeks for the vaccine to produce an effective response in the body.
Ongoing Now: 2022 – 2023 Influenza Season
October 14, 2022: Early increases in seasonal influenza activity have been reported in most of the United States, with the southeast and south-central areas of the country reporting the highest levels of activity (CDC FluView Tracker). Highest activity is reported in Georgia, New York City, South Carolina, Tennessee, Texas, Virginia, and Washington D.C.
The majority of viruses detected, to date, are Influenza A (H3N2). There is currently no pregnancy-specific data yet for this current season (CDC FluView Tracker).

Past Flu Seasons
2021 – 2022
The severity of the 2021–22 influenza season was low, with two waves of influenza A activity. The overall burden of influenza for the 2021-2022 season was an estimated 9 million flu illnesses, 4 million flu-related medical visits, 100,000 flu-related hospitalizations, and 5,000 flu deaths.
Compared with influenza seasons prior to pandemic, the 2021–2022 influenza season was mild and occurred in two waves, with a higher number of hospitalizations in the second wave. Influenza activity in the United States during the 2021–2022 season began to increase in November, declined in January 2022, increased again in March 2022 and remained elevated until mid-June 2022. Pregnancy specific data is not yet available.
2020 – 2021
According to the CDC (which tracks this data), flu activity was unusually low throughout the 2020-2021 flu season both in the United States and globally, despite high levels of testing. During September 28, 2020–May 22, 2021 in the United States, 1,675 (0.2%) of 818,939 respiratory specimens tested by U.S. clinical laboratories were positive for an influenza virus. The low level of flu activity during this past season contributed to dramatically fewer flu illnesses, hospitalizations, and deaths compared with previous flu seasons.
COVID-19 mitigation measures such as wearing face masks, staying home, hand washing, school closures, reduced travel, increased ventilation of indoor spaces, and physical distancing, likely contributed to the decline in 2020-2021 flu incidence, hospitalizations and deaths. Pregnancy-specific data is not yet available.
2019 – 2020
According to preliminary statistics reported by the CDC, from October 1, 2019 to April 4, 2020, there was an estimated 38 million influenza illnesses, 405,000 hospitalizations, and 22,000 deaths. CDC provides large estimate ranges since not all cases of influenza will be formerly diagnosed or reported.
According to the CDC, the season was characterized by two consecutive waves of activity, beginning with influenza B viruses and followed by A(H1N1) viruses. Overall, influenza A(H1N1) viruses were the most commonly reported influenza viruses. Activity began to decline in March.
It is possible that social distancing efforts during February to April 2020 had a beneficial impact late in the season on influenza infection rates.
Further, CDC reported the number of hospitalizations estimated during this season was lower than end-of-season total hospitalization estimates for any season since CDC began making these estimates.
Pre-Pandemic: 2018 – 2019
Although limited information is available, influenza activity in the U.S. during the 2018–19 season was considered of moderate severity; activity began increasing in November, peaked in mid-February, and returned to baseline in mid-April (considered the longest season of the last ten years).
As of June 13, 2019, data were available for 6,399 hospitalized adults; among 759 hospitalized females aged 15–44 years with information on pregnancy status, 152 (28.7%) were pregnant.
Action
Not all pregnant women who contract influenza will have serious illness. However, there is currently no way to determine which women may experience a more severe course of the disease.
Current research indicates, to date, the best way women can protect themselves and their babies during pregnancy is to practice good hygiene, wash their hands, get vaccinated, and call their HCPs immediately when they have a fever or believe they may have the flu.
Pregnant women are also advised to see their HCP immediately or call 911 if they experience:
Difficulty breathing or shortness of breath
Persistent pain or pressure in the chest or abdomen
Persistent dizziness, confusion, inability to arouse
Seizures
Not urinating
Severe muscle pain and/or weakness
Fever or cough that improves but then returns or worsens (may indicate pneumonia)
High fever that is not responding to acetaminophen or other anti-fever medication
Women should also consider sharing and submitting their experience below regarding influenza during pregnancy.
Partners/Support
Due to the possible severe complications that can occur when a pregnant woman contracts influenza, partners/support members have a role in the prevention of the spread of the infection, as well as assisting in the early identification of signs/symptoms in pregnant women.

Partners/support should begin by reading the above information regarding influenza and pregnancy. Early recognition of symptoms, diagnosis, and treatment can help prevent serious illness and complications in both the mother and baby.
Partners can help women recognize when they may be ill, have a fever, or should call their HCP. While not all pregnant women who contract influenza will experience a severe form of illness, partners/support may be especially critical if the woman starts to experience sudden severe illness.
Partners/support can lessen the risk of spread by: getting vaccinated, limiting their contact with others who may spread the infection during influenza season, washing their hands, regularly cleaning surfaces, and encouraging other family members to not only do the same, but to get vaccinated as well.
Resources
Assessment and Treatment of Pregnant Women With Suspected or Confirmed Influenza (American College of Obstetricians and Gynecologists)
Pregnant Women and Influenza Vaccinations (U.S. Centers for Disease Control and Prevention)
Flu Season Updates (U.S. Centers for Disease Control and Prevention)