Umbilical Cord
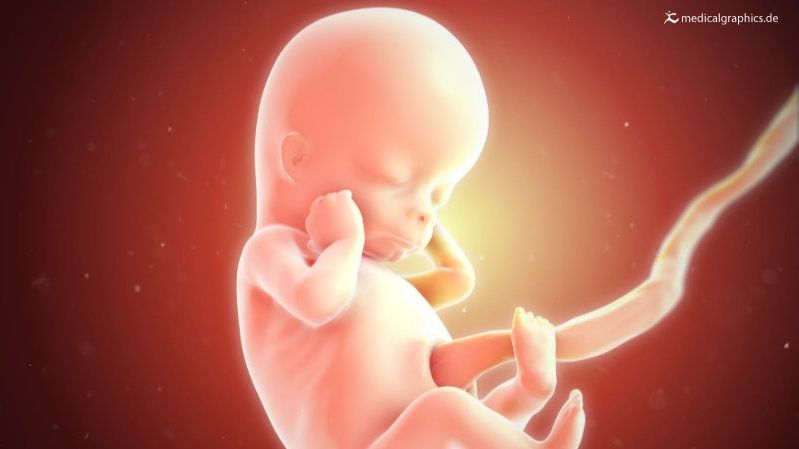
The umbilical cord physically connects the fetus to the placenta, begins to develop early in pregnancy, and is complete by 12 weeks. The cord plays an important role in the transfer of nutrients to the fetus and the transfer of waste away from the fetus (and to the placenta).
The umbilical cord can vary in length and diameter depending on a variety of factors and can possess characteristics such as blood vessel abnormalities, loops, knots, and cysts, which do not always lead to complications.
Most of these characteristics are found after delivery, as the entire length of the umbilical cord can be hard to visualize during ultrasound assessments.
Women should read below for more information regarding various aspects of the umbilical cord, to include delayed clamping and cord blood banking.
Background
Graphic warning: A photograph of a real placenta and umbilical cord is located in the section "Length and Diameter".
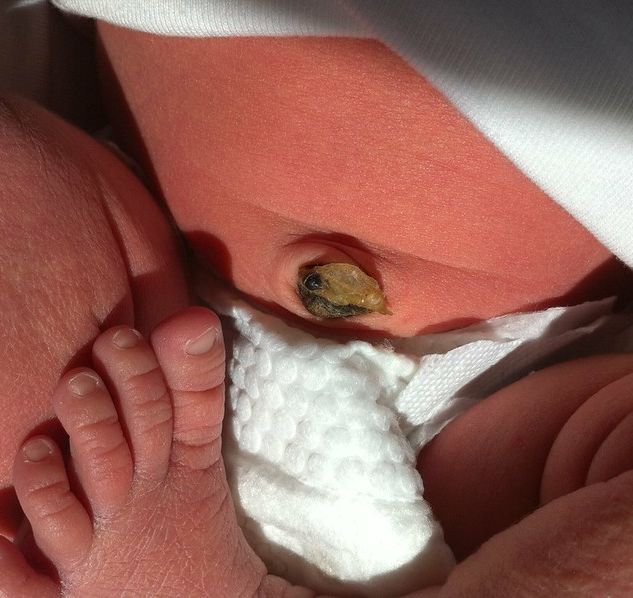
After delivery, the cord is clamped and cut; the stub that remains on the newborn’s abdomen falls off after a couple days.
Assessment of the umbilical cord is done during ultrasound examinations and is considered a critical feature to evaluate. The cord is assessed for length, diameter, insertion, entanglements, knots and coils. However, it can be difficult to see the entire cord based on the positioning of the fetus. Therefore, most umbilical cord abnormalities are usually found after delivery when the cord is examined.
Blood Vessels
The fully developed umbilical cord contains two arteries and one vein. The vein caries oxygen and nutrients from the placenta to the fetus, while the arteries take low-oxygenated blood and waste from the fetus to the placenta; the waste is then transferred to the woman’s blood and filtered through her kidneys.
These blood vessels are protected within the cord by a cushioning gelatin-like substance known as Wharton’s jelly.
About 1% of single pregnancies and 5% of multiple pregnancies have an umbilical cord that contains only two blood vessels, instead of the normal three (one artery is missing), the cause of which is unknown.
Blood flow through the umbilical vessels is usually assessed by Doppler ultrasound. If an artery is deemed missing from the umbilical cord, women are offered the option of various screening and diagnostic tests to confirm or rule out birth defects.
However, studies are inconsistent regarding whether fetuses with a single umbilical artery may have an increased risk for certain birth defects, such as heart, central nervous system, or urinary tract abnormalities.
It has been estimated that by 31 weeks, the umbilical cord must carry 70 quarts of blood per day, moving at 4 miles an hour.
Length and Diameter
Cord length becomes progressively longer until 28 weeks of pregnancy and generally coils around itself. At term, the umbilical cord has an average diameter of 8 to 20 millimeters (mm) or 2 centimeters (cm) and a length of 50 to 60 cm, but can range from 30 to 100 cm.
The normal umbilical cord has one coil per 5 cm of cord length and may contain up to 40 spirals in different directions.
This image contains triggers for: Blood, Internal Anatomy, Real Delivery
You control trigger warnings in your account settings.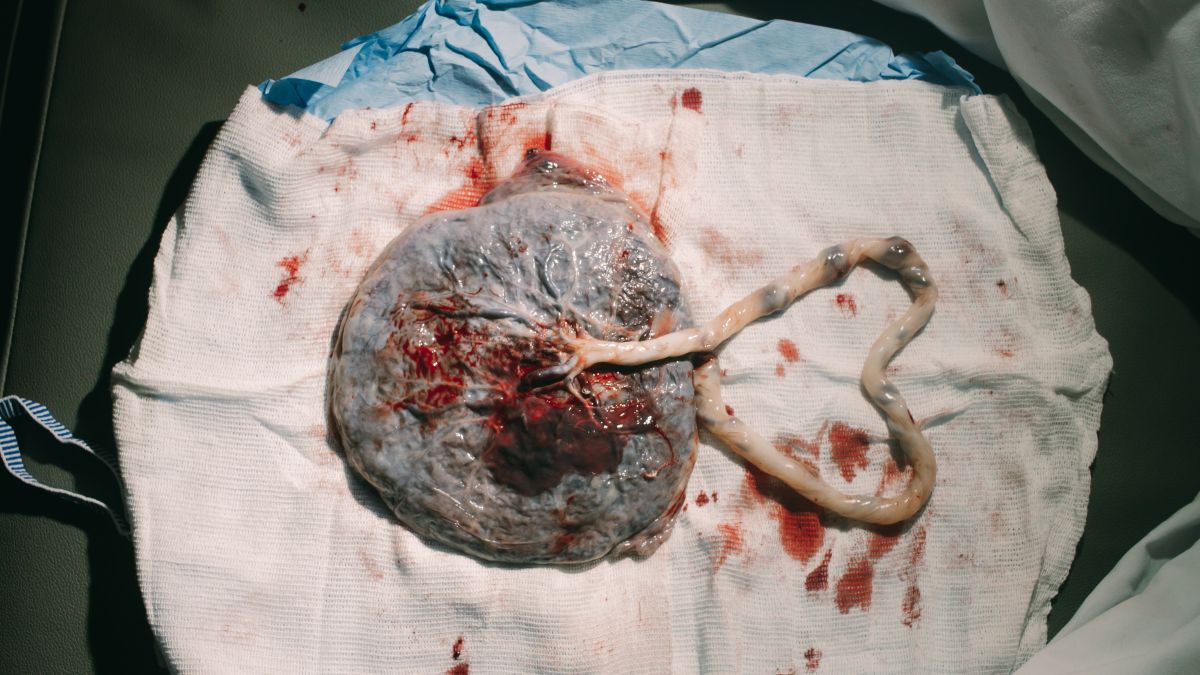
Although disputed, the “stretch hypothesis” indicates that tensile force is an important determinant for cord length, thereby suggesting that an active fetus develops a longer cord.
It is also assessed that cord length may be longer in male fetuses (who also tend to be more active), and that these differences may start to appear around 27 weeks.
The length of umbilical cords was studied in 536 term deliveries to test the hypothesis that a short or long umbilical cord is more frequently associated with certain complications. The mean umbilical cord length was 55 cm (range, 14 to 129 cm). A short cord was defined as 35 cm or less. Umbilical cord complications were most frequent in the presence of a long cord.
Excessively long cords may be associated with prolapse, looping of the cord around the fetal neck, entanglement, distress, and fetal demise.
Similarly, very short cords may be associated with delayed fetal descent, premature placental separation, growth restriction, congenital abnormalities, fetal distress, and demise.
Prolapse
Umbilical cord prolapse occurs when the cord slips into the vagina after the membranes (bag of waters) have ruptured, and before the baby descends into the birth canal; prolapse is estimated to affect 1 in 300 births. If not managed quickly, prolapse can lead to severe complications.
While the cord is in the vagina, the baby passes through the cervix and into the vagina during delivery, putting pressure on the cord and cutting off its blood supply.
Umbilical cord prolapse can result in stillbirth unless the baby is delivered immediately – usually through cesarean section. Prolapse is normally identified during vaginal examination, or when monitoring of the fetal heart rate shows abnormal patterns during delivery.
Note: During the time between diagnosis and cesarean section, HCPs may try different maneuvers to further prevent both cord compression and cord prolapse beyond the vagina (e.g. knee-chest position). However, "each maneuver has its own advantages and limitations; thus, they should be applied wisely and with great caution, depending on the actual clinical situation".
Nuchal Cord (Loop)
About 25% of babies are born with a nuchal cord (the umbilical cord wrapped around the baby's neck). The overall rate of adverse outcomes, or if a tight cord affects outcomes at all, is debated.
A nuchal cord, also called a nuchal loop, is not a problem in the majority of deliveries – even tight cords, but can depend on the degree of cord blood vessel compression (assessed to be rare).
If distress is concerning enough, cesarean delivery may be needed, although even this is debated; the true incidence of cesarean delivery due to a tight nuchal cord is not known.
True and False Knots
Twisting, bending, looping, and sometimes knotting is common with the umbilical cord because the umbilical cord vessels inside are longer than the cord itself. Knots can be formed when the loops occur and the baby moves through the loop creating a knot.
True knots are usually developed in the first trimester, when the cord is long and the fetus is small enough to move around more.
False knots ("looser knot" or suspected knot) are believed to have no significance during pregnancy and cause no concerns. The main concern is a true knot, which can tighten and cause severe complications.
However true knots are very rare (from less than 1% to 2% of pregnancies), and are not always life-threatening; not every true knot is tight enough to cause problems. It estimated that of the less than 1% of true knots that occur, only 5% of those result in stillbirth.
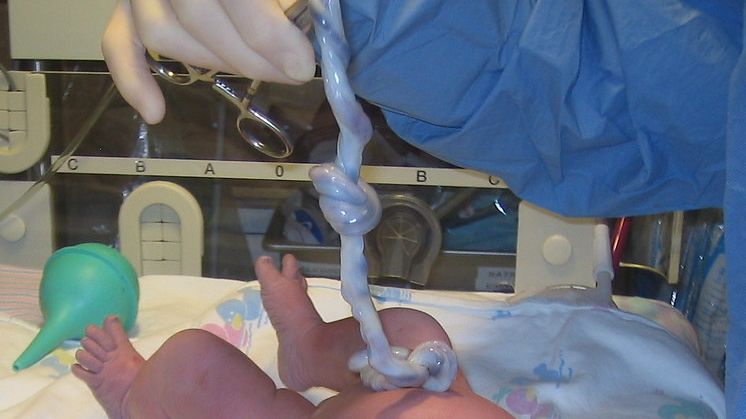
True knots are usually discovered after delivery. During delivery, the baby’s heart rate is monitored. Any tight, undiagnosed knot that causes changes to the baby’s heart rate during labor will likely result in a cesarean section, which prevents furthering tightening. Other knots are loose enough to not cause problems during labor and delivery and are only discovered after inspection of the umbilical cord. Apgar scores in these cases are usually normal.
The strongest risk factor for a cord knot is a long umbilical cord. Further, knots are more strongly associated with male fetuses. Males tend to have longer cords and are usually more active during pregnancy, which increases the risk of a knot.
Additional risk factors include an excess of amniotic fluid, small size of the fetus, gestational diabetes, carrying multiples, twins that share one amniotic sac, amniocentesis, a prolonged pregnancy, and chronic high blood pressure.
The most common symptom of a true knot is reduced fetal activity after 37 weeks. Fetal monitoring by the mother can potentially raise a flag in the rare event a true knot does occur.
Knots are difficult to prevent/manage. If a knot is seen prior to delivery, Doppler ultrasound may be used to assess and monitor blood flow.
Cysts
Like knots, there are true and false cysts. True cysts are lined with cells and generally contain remnants of early embryonic structures, while false cysts are fluid-filled and are related to a swelling of the Wharton’s jelly.
Umbilical cord cysts are found in about 3% of pregnancies, and only about 20% of these are associated with fetal abnormalities.
However, there does not appear to be an association between negative outcomes and a single umbilical cord cyst during the first trimester, if all other assessment data is normal, and the cyst is not seen on a follow-up ultrasound (most cysts in the first trimester resolve on their own).
However, pregnancy complications are more likely if the cyst is located within a few cm of the placenta or fetus, if the cyst remains beyond 12 weeks' gestation, or if there is more than one. Possible defects may include chromosomal abnormalities or abdominal wall defects.
When a cord cyst is found during an ultrasound, an HCP may recommend additional tests, such as amniocentesis and a detailed ultrasound, to diagnose or rule out birth defects. If additional tests are normal, then the cyst(s) may not have any significance.
Delayed Clamping
There is current debate whether early or delayed cord clamping is preferable after delivery.
Active management of labor, or purposeful action that actively moves labor along, includes immediate cord clamping which is thought to reduce the risk of postpartum hemorrhage.
Delayed cord clamping involves waiting for several minutes after delivery before clamping, which allows a larger placental transfusion of oxygenated blood into the newborn.
The extra blood transfusion may have benefits for the baby:
It has been reported that 80 to 100 milliliters of blood transfers from the placenta to the newborn in the first 3 minutes after birth, supplying the baby with extra iron that may help prevent iron deficiency for the entire first year of life.
A term newborn held 10 cm below the level of the uterus during the first three minutes of life increases its blood volume by an average of 32%.
It is also possible that delayed clamping facilitates the transfer of immunoglobulins and stem cells, essential for tissue and organ repair.
The American College of Obstetricians and Gynecologists recommends a delay in umbilical cord clamping in healthy term and preterm infants for at least 30 to 60 seconds after birth. The American College of Nurse–Midwives recommends delayed umbilical cord clamping for 2 to 5 minutes after birth.
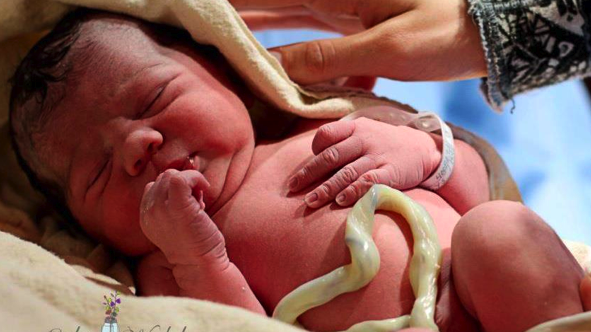
It has also been recommended that newborns be held lower than the uterus in order to use gravity to assist the transfusion, but placing the newborn on the mother’s chest appears to have the same effect, and therefore, if desired, immediate skin-to-skin should not be withheld for the purpose of clamping.
Delayed cord clamping can also occur with cesarean sections. The baby can be placed on the mother’s abdomen or legs or held by the surgeon close to the level of the placenta until the cord is clamped.
Many of the clinical trials that evaluated delayed umbilical cord clamping did not include multiple gestations; therefore, information on the effectiveness or safety of delayed clamping on twins or higher is not completely known.
There are situations in which delayed clamping is not recommended, such as when immediate lifesaving or resuscitation efforts are needed for the newborn, or there are concerns with the placenta.
There is no evidence that delayed clamping by one or two minutes increases the risk of postpartum hemorrhage or increased blood loss at delivery. However, if a woman has risk factors for heavy bleeding after delivery, the risks and benefits of delayed clamping vs. the possibility of hemorrhaging needs to be discussed with an HCP.
Additional concerns/considerations with delayed umbilical cord clamping is the possibility of excessive placental transfusion, respiratory symptoms, polycythemia (excess red blood cells), hyperbilirubinemia (too much bilirubin in the blood), and jaundice, but these links are not very strong.
Cord Blood
Cord blood contains blood-forming stem cells that can be used in the treatment of patients with blood cancers such as leukemias and lymphomas, as well as certain disorders of the blood and immune systems. Cord blood is approved only for use in individuals with disorders affecting the blood forming system.
It is possible that delayed clamping can decrease the amount of blood available for cord blood blanking. If parents wish to collect cord blood, as well as a delayed clamping, a risks and benefits discussion needs to occur with an HCP.
Action
Current research indicates that a nuchal cord or knot likely does not affect pregnancy outcome or delivery mode, but needs to be assessed on an individualized basis at the discretion of the woman's HCP.
Women with concerns or questions regarding nuchal cords or knots, especially if found or assessed during an ultrasound exam, need to have a discussion with their HCP (to include risks and benefits of possible management, if necessary).
Resources
Umbilical Cord Care - Newborn (Children's Hospital of Philadelphia)