Ultrasound

Ultrasounds are commonly used in obstetrics. Most women will receive two to three of these examinations during their pregnancy, sometimes more if monitoring is required.
Although some safety concerns have been raised regarding the possibility of fetal tissue heating/hearing effects with the use of ultrasound, there is no current evidence indicating ultrasound is harmful when used appropriately.
However, newer ultrasounds do not have the established safety profile of traditional ultrasound machines, so most organizations recommend that ultrasounds be used for medical assessment only and for the shortest time necessary.
This recommendation does not indicate that ultrasound is a concern; utilizing any medical technique or treatment for the shortest time necessary is the best way to eliminate any unknown or immeasurable amount of risk, even if only theoretical.
Women should continue reading to learn how ultrasound works, when and why it is used during pregnancy, and what ultrasound can tell HCPs regarding the health of their pregnancy.
Background
One of the most common uses of ultrasound in all of medicine is to monitor the growth and development of a fetus. Ultrasound is painless and quick – and as a screening tool – provides immediate results (confirmation is done through additional testing).
Sound at a vibration rate greater than 20,000 cycles per second is called ultrasound (no radiation). A wand known as a transducer emits ultrasound waves through tissues to detect their distance from the wand to create a visual picture. Transducers produce sound waves with frequencies above the threshold of human hearing.
Types of Ultrasound
A transvaginal ultrasound may be used when a woman is earlier than 8 weeks pregnant. This type of ultrasound is done by placing a lubricated wand about the size of a finger gently into the vagina while the woman lies on her back. The wand is then moved around slightly.
This method allows for more detailed imaging in early pregnancy and can show intrauterine structures approximately one week earlier than transabdominal ultrasound. It is performed with an empty bladder which allows for more accurate assessment.
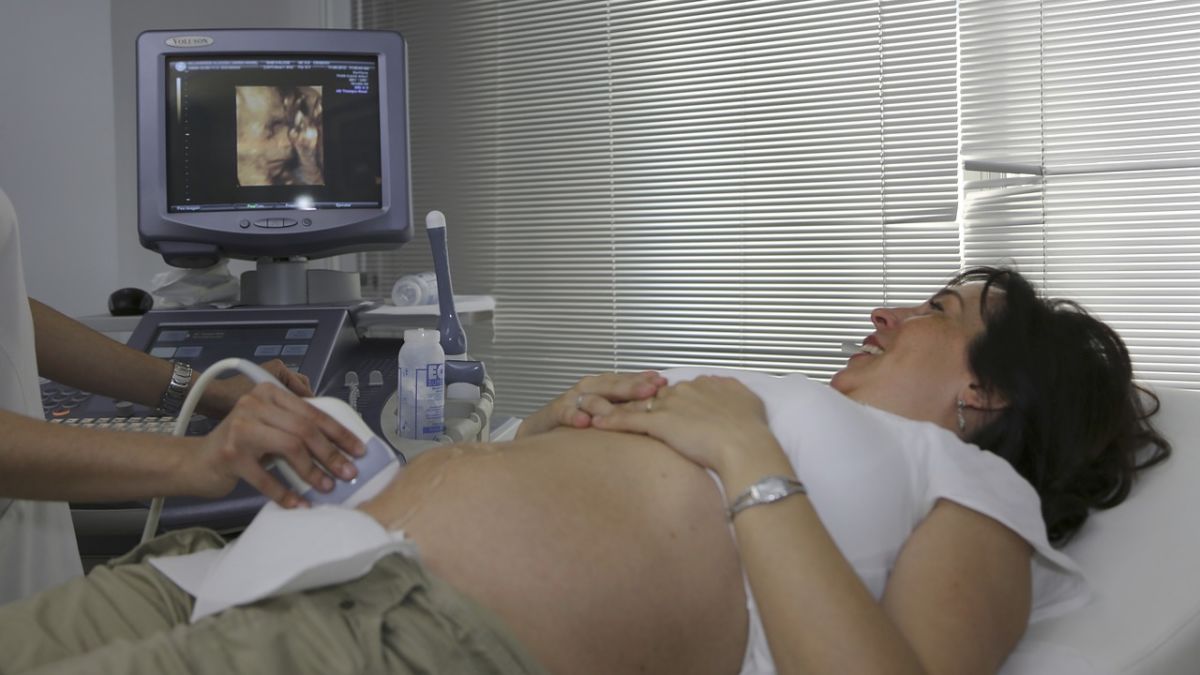
The most well-known type of ultrasound is transabdominal. In transabdominal ultrasound, a woman lies on her back, and a technician places a thin layer of warm gel on her abdomen and moves a wand over the gel to create a visual on the screen. For this type of ultrasound, a full bladder is preferred, so it can be used as a reference point.
Doppler ultrasound is considered a functional type of ultrasound as it is used to assess blood flow in vessels within the body, heart, and umbilical cord.
A 3D ultrasound looks and feels like transabdominal, but the technology is different. A 3D ultrasound takes thousands of pictures at once which are used to create a 3D image of the fetus and can be useful for more detailed screening. A 4D ultrasound can show fetal movements in video form.
Screenings
Most women, depending on the practice, will have two to three ultrasounds during pregnancy.
Dating scan (usually transvaginal): 6 to 8 weeks of pregnancy to confirm a pregnancy, due date, check early growth, and determine the possibility of twins or more (a follow up ultrasound may occur 1 to 2 weeks later; see First Trimester Viability).
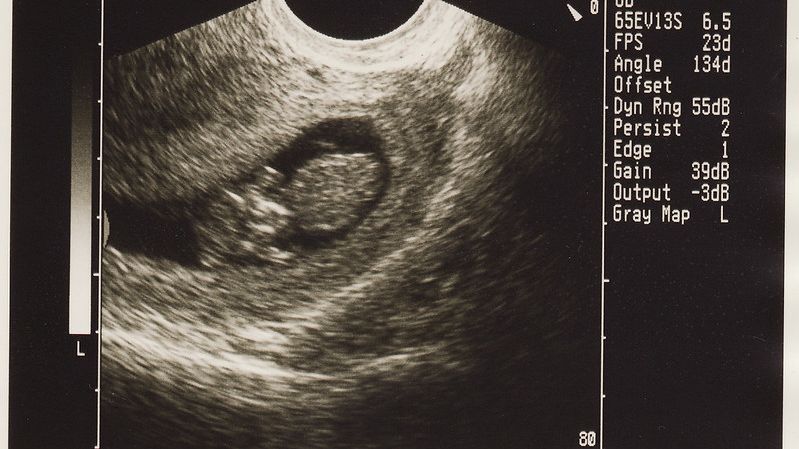
First trimester (transabdominal): 12 to 13 weeks (for some women, this may be their first scan); the purpose of this ultrasound is to:
Confirm a pregnancy
Confirm the pregnancy is viable (and rule out ectopic or molar pregnancy)
Assess a fetus’ growth and development
Determine a due date
Check for multiples
Screen for birth defects
Assess if bleeding is present or attempt to determine a cause of bleeding
Second Trimester (transabdominal): known as the anomaly scan, occurs between 18 and 22 weeks when more anatomical details are present (usually a woman’s second scan); the main purpose of this scan is to screen for potential birth defects by observing, assessing, and measuring anatomical details to include the placenta and amniotic fluid.
Third Trimester (transabdominal): most women will not require a third trimester scan, but some practices may perform one to check the baby’s position, amniotic fluid levels, cervical length, or fetal movement.
The biggest risk in the use of ultrasound is not necessarily a safety concern, but the risk of misdiagnosis. Ultrasound is a screening tool that attempts to determine level of risk based on initial visual assessment.
If a potential complication or birth defect is suspected, additional testing – known as diagnostic tests – are the next step. Ultrasounds are very useful in identifying birth defects, but they can also raise the possibility of a birth defect that is not actually present. Regardless, ultrasounds are used as a first step because they are safer than diagnostic tests, which may carry a small risk of complications when they are performed.
Safety
Ultrasound use in obstetrics has increased dramatically in recent years, mostly through private use of women booking time to find out the sex of the baby or to collect additional photographs and video. The main reason for most of this additional use is the widespread acceptance of the safety of ultrasound.
It is currently assessed that ultrasound use for obstetric reasons is free of risk from any ultrasound-induced bioeffects. However, although research into the bioeffects of ultrasound has been studied for decades, there are no well-designed studies regarding the effects of ultrasound on pregnant animals or humans because these potential effects are very difficult to assess.
Nevertheless, there is also no current reason to suspect, based on what is already known about ultrasound, that it should be a concern during pregnancy.

As ultrasound travels through tissue, energy is absorbed by the tissue and is converted to heat. It is theoretically possible that newer ultrasound machines can produce heat in fetal tissue – under the worst conditions – but there is currently no link from research completed to date. Additionally, this would require a lengthy ultrasound exam focused on one tissue specifically, and most modern machines have safety controls to prevent excessive power output and dwell time.
Currently, there is no evidence that ultrasound is harmful to a developing fetus. No links have been found between ultrasound and birth defects, childhood cancer, or developmental problems. There is also no evidence that ultrasound is harmful to fetal hearing.
Despite the above, the U.S. Food and Drug Administration, the American College of Obstetricians and Gynecologists, and the American Institute of Ultrasound in Medicine do not recommend non-medical use of ultrasounds for the purpose of additional keepsakes. Utilizing any medical technique or treatment for the shortest time necessary is the best way to eliminate any unknown or immeasurable amount of risk, even if only theoretical.
Note: Doppler ultrasound may increase potential heating risk further than standard ultrasound, as it produces high-energy acoustic outputs. It is recommended Doppler ultrasound should also only be applied when needed and within the shortest time possible.
Fetal Sex Determination
Sex identification of a fetus is normally determined between 18 and 22 weeks of pregnancy via ultrasound during the anomaly scan. Although technology is improving quickly, it is not yet possible to accurately and reliably observe external genitalia in the first trimester – even with 3D ultrasound. Correct identification is also dependent on the ultrasound technician, machine, and fetal position.

Fetal sex determination via ultrasound is most accurate, and best identified after at least 14 weeks of pregnancy (read Reproductive System).
Although debated, some research indicates that first trimester identification can be done from 11 weeks of pregnancy using the direction of the genital tubercle:
The genital tubercle is a tissue of the reproductive organs that is positioned differently depending on the sex of the fetus that will eventually develop. It either elongates to become the penis or grows very minimally to be the clitoris. The downward direction of the tubercle is considered a female while the upward direction is considered male.
Another commonly held belief is the female fetus has a more rapid heart rate than the male fetus, and the early rate can be used to attempt to determine the sex of the fetus. Numerous studies refute this belief, indicating there are no significant differences between heart rates of male or female fetuses, and certainly not enough difference as a reliable way to determine fetal sex.
Actions
Women who have any questions or concerns regarding ultrasounds or their results need to have a discussion with their HCP if there is something they do not understand.
As a general rule, ultrasound technicians are not allowed to give results to any patient, and must wait until the results are reviewed by the HCP or radiologist, who have more training in the interpretation of the images.
Resources
Detailed Anatomy Example Images (American Institute of Ultrasound in Medicine)
Ultrasound Examinations (American College of Obstetricians and Gynecologists)
Practice Parameter for the Performance of Standard Diagnostic Obstetric Ultrasound Examinations (AIUM-ACR-ACOG-SMFM-SRU)
Practice Parameter for the Performance of Detailed Second- and Third-Trimester Diagnostic Obstetric Ultrasound Examinations (American Institute of Ultrasound in Medicine)
Short video on how ultrasound works (U.S. National Institutes of Health)