Radiation
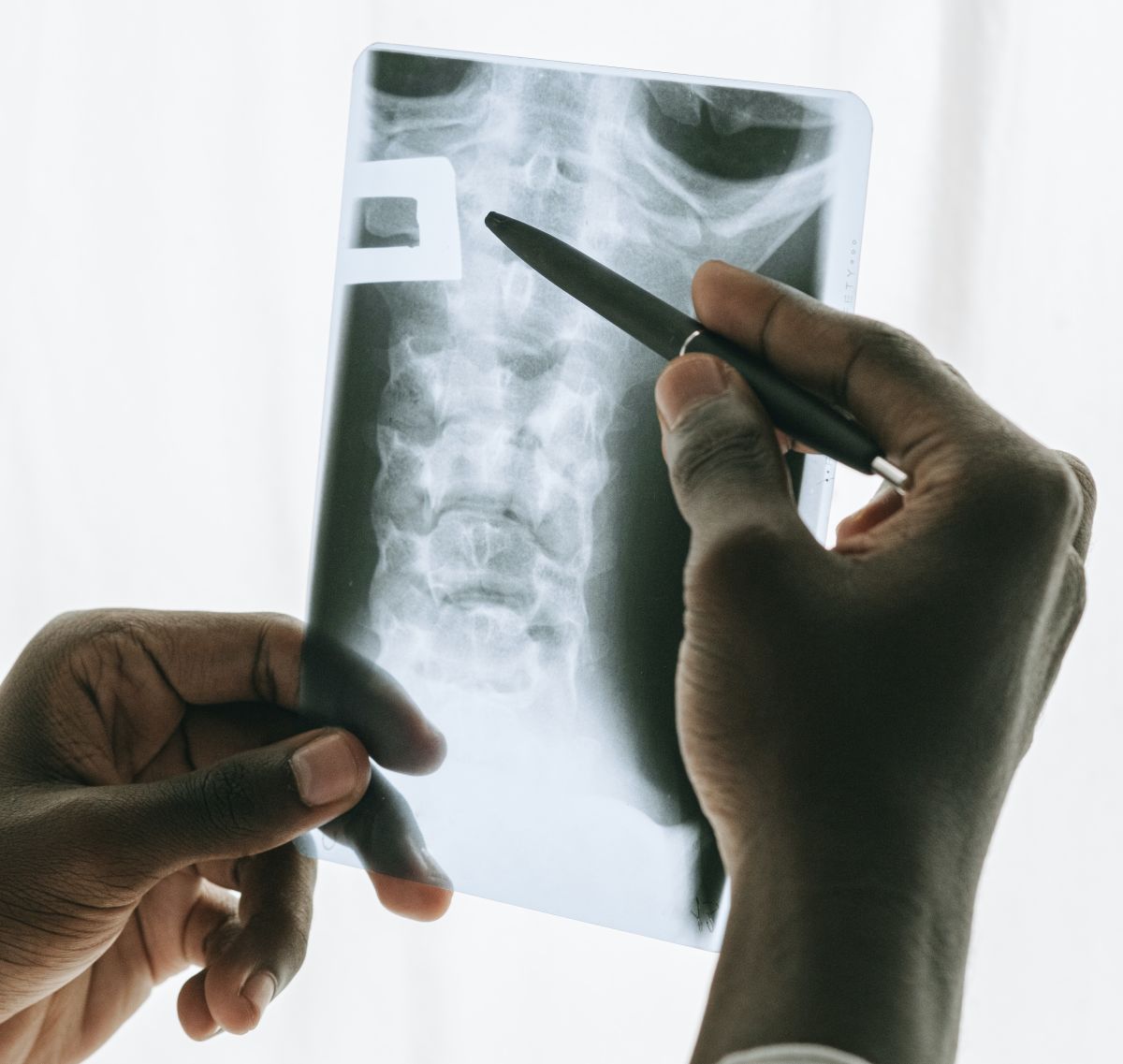
It is possible that some women will require diagnostic imaging during pregnancy due to a broken bone or other injury, abdominal, back, or pelvic pain, or other symptoms that require ruling out possible diseases or conditions.
Pregnant women usually require diagnostic medical imaging at a similar rate to non-pregnant individuals. Fortunately, depending on the indication for it, ultrasound and MRI are usually recommended first, neither of which use ionizing radiation.
If a pregnant woman requires an imaging technique such as an x-ray or CT scan, which do use radiation, the exposure dose for a single scan to the embryo/fetus is estimated to be almost negligible.
However, the dose and potential risk to the embryo or fetus depends on the stage of pregnancy, dose used, type of scan, and what the scan is imaging. For example, radiation exposure from an x-ray of the hand or foot with a lead shield over the abdomen is estimated to pose almost no risk of exposure to the fetus.
Any pregnant woman requiring an image during pregnancy that uses radiation should have a risks and benefits discussion with her HCP. There are numerous scenarios in which the valuable medical information that will be evident from an imaging scan may outweigh any potential risk to the fetus.
Background
Radiation is a type of energy that travels as rays or particles in the air. When used for medical imaging, these rays are used to pass through the body to create an image.
Ionizing radiation: radiation with enough energy so that during an interaction with an atom, it can remove tightly bound electrons from the orbit of an atom, causing the atom to become charged or ionized; used in x-rays, CT scans, and nuclear medicine procedures.
Non-ionizing radiation: a series of energy waves composed of oscillating electric and magnetic fields traveling at the speed of light; these waves do not have enough energy to cause ionization; includes the spectrum of ultraviolet (UV), visible light, infrared, microwave, radio frequency, and extremely low frequency (i.e. cell phone).
It is estimated that about 25% of pregnant women have had an imaging experience during pregnancy, either for obstetrical reasons or during medical or dental examinations. This number is increasing, especially for CT procedures.
Confusion about the safety of various imaging techniques during pregnancy leads some women to avoid necessary diagnostic tests. The risks from radiation exposure due to x-ray or CT scan is highly dependent on various factors described in detail below (see Timing and Exposure).
Additionally, the environment can be adequately controlled to prevent as much exposure as possible while still obtaining an adequate image.
Imaging Types – Overview
The most common imaging techniques during pregnancy:
Ultrasound: uses ultrasound to generate an image (no radiation); women may receive two to three of these examinations throughout their pregnancy, sometimes more if monitoring is required. Read more.
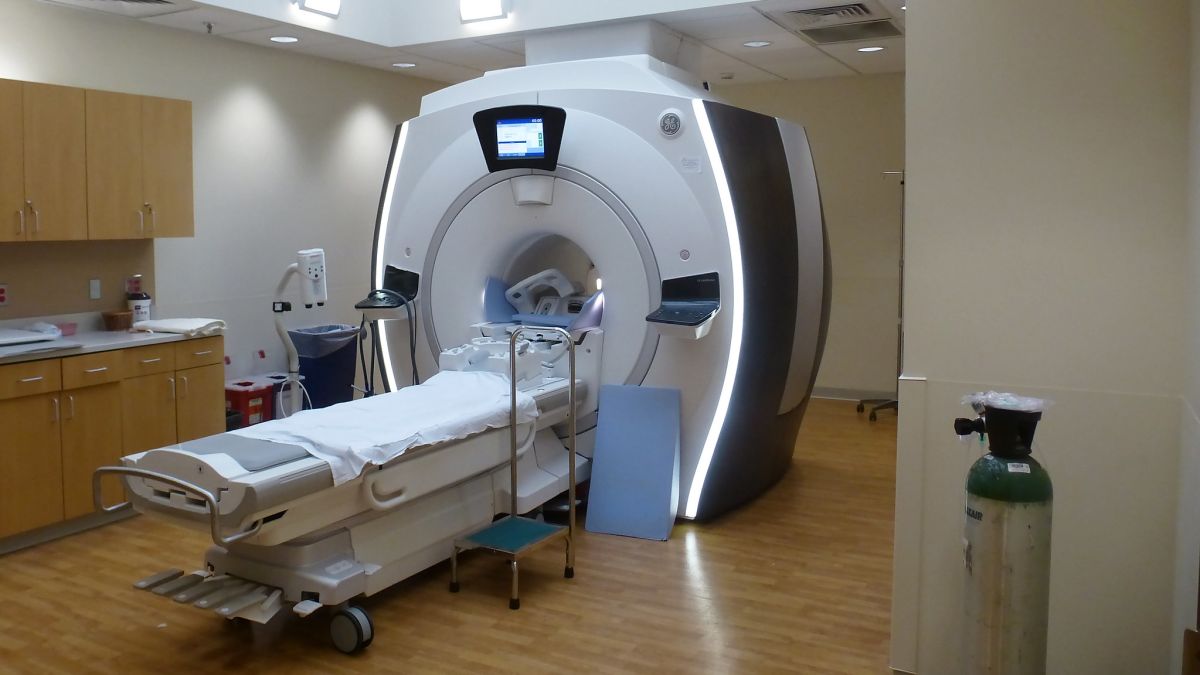
Magnetic resonance imaging (MRI): uses a powerful magnetic field, radio waves, and a computer to produce detailed pictures; shows detailed imagery of blood vessels, bones, organs, lymph nodes, and connective tissue (no ionizing radiation).
X-ray: uses a very small dose of ionizing radiation to produce pictures of bone; most commonly used to diagnose fractures and joint injuries (ionizing radiation).
Computed Tomography (CT or CAT) scan: uses ionizing radiation to produce images of internal organs, bones, soft tissues, and blood vessels; usually used in an emergency, such as trauma; it can reveal internal injuries and bleeding very quickly (an MRI can take 30 minutes or longer).
The principal imaging techniques during pregnancy are ultrasound and MRI, neither of which use ionization radiation, nor have any documented adverse effects during pregnancy. These are the first-line imaging techniques of choice during pregnancy.
There may be many different reasons pregnant women require a diagnostic test that uses radiation. Severe injury, orthopedic injury, trauma, and suspected malignancy, appendicitis, kidney stones, and/or gallstones are some of the most common. For any image request during pregnancy, women need to have a risks and benefits discussion with their HCP regarding general concerns, the necessity of the test, risks in performing the scan, as well the risks in not performing the scan.
Timing and Exposure – General
The possible effects of fetal radiation exposure include prenatal death, intrauterine growth restriction, small head size, mental disabilities, birth defects, and childhood cancer.
However, radiation risks throughout pregnancy are related to the stage of pregnancy, the absorbed dose, the amount of tissue the x-ray beam must penetrate, the direction of the projection, the depth of the embryo/fetus from the skin surface, x-ray technique factors, and lead shielding. Not all types of imaging expose the fetus to the same dose or in the same way.
Additionally, scatter radiation is considered so minimal that lead shielding may provide more reassurance than actual protection.
Diagnostic x-ray studies that may involve direct radiation exposure to the early developing embryo include:
X-rays of the back
X-rays to examine kidney function
Upper GI series (gastrointestinal assessment)
Lower GI series (barium enema)
X-ray studies of bladder
X-ray studies of the gallbladder
X-ray studies of the structure and function of the uterus and tubes
X-ray studies of the pelvis and hips
Standard abdominal x-rays
When a diagnostic x-ray study is of the head, teeth, chest, arms, neck, or legs, the radiation exposure is not to the embryo or ovaries; although scatter may reach the embryo, this is estimated to be too small to pose any risk to the embryo; any other imaging is kept at the lowest dose that will still reasonably achieve the necessary image.
According to the American College of Radiation, no single diagnostic x-ray has a radiation dose significant enough to cause adverse effects in the developing embryo or fetus.
Fetal Exposure
It is assessed that during the first two weeks after fertilization (3 to 4 weeks of pregnancy), the embryo is very resistant to the adverse effects of x-rays. However, there is a risk of pregnancy loss at high exposure, approximately 150 mGy. Data from animal studies indicate the risk of loss at this stage increases between 0.5% and 1% per 10 mGy. However, embryos that survive radiation exposure at this stage appear to develop normally (known as the "all-or-none-phenomenon".
It is assessed that from 4 to 8 weeks of pregnancy – a period of fast organ development – the embryo is not substantially affected enough to cause birth defects, miscarriage, or growth restriction unless exposure is substantially above 100 milligrays (mGy).
Several other reviews indicate the risk of fetal anomalies, growth restriction, or pregnancy loss is not assessed to be increased with radiation doses of less than 50 to 150 mGy.
From 8 to 15 weeks of pregnancy, the embryo or fetus is most sensitive to the effects of radiation on the central nervous system, but likely only around an exposure of at least 50 mGy, in which effects on IQ may be seen. General diagnostic studies do not reach these levels and may therefore be of negligible concern during pregnancy.
CT pelvic exposure can be as high as 50 mGy, but can be reduced to approximately 2.5 mGy through a low-exposure technique that is adequate for diagnosis. Fetal doses of 100 mGy are not reached even with 3 pelvic CT scans or 20 conventional diagnostic x-ray examinations.
In general, fetal radiation doses from radiographic, fluoroscopic, and CT examinations of the abdomen and pelvis and from nuclear medicine studies rarely exceed 25 mGy. The estimated fetal radiation dose from one head CT is less than 10 mGy (1 rad).
The estimated fetal dose from chest radiographs is less than 0.01 mGy. By comparison, the fetal dose during a transatlantic flight is 0.01 mGy, and naturally occurring background radiation during pregnancy is 1 mGy.
If abdominal trauma or other condition or injury is suspected, the benefits of an abdominal or pelvic CT scan may outweigh possible risks to the fetus.

However, any exposure above zero can theoretically increase the risk of adverse effects, but the minimum amount at which these effects start to appear is not known. Risk is very hard to assess, and different researchers have concluded different increases in risk.
At least one study noted that while approximately 1 in every 500 children develops cancer during childhood even in the absence of radiation exposure, it is estimated that for a fetus exposed to one of the highest doses of radiation from a diagnostic test after the first 4 weeks, the risk of childhood cancer might be increased to 3 in 500. Further, a 10–20 mGy fetal exposure may increase the risk of leukemia by a factor of 1.5–2.0 over a background of ~1 in 3000.
Policy guidelines:
According to a statement published by the International Commission on Radiological Protection: “Prenatal doses from most properly done diagnostic procedures present no measurably increased risk of prenatal death, malformation, or impairment of mental development over the background incidence of these entities".
In 1977, the National Council on Radiation Protection and Measurements (NCRPM) issued the following statement: “The risk [of abnormality] is considered to be negligible at 50 mSv [mSv = mGy] or less when compared to other risks of pregnancy, and the risk of malformations is significantly increased above control levels only at doses above 150 mGy”; the NCRPM recommended maximum dose during pregnancy is 50 mGy (5 rad).
More recently, the American College of Obstetricians and Gynecologists (ACOG) published the following policy statement: “Women should be counseled that x-ray exposure from a single diagnostic procedure does not result in harmful fetal effects. Specifically, exposure to less than 50 mGy (5 rad) has not been associated with an increase in fetal anomalies or pregnancy loss".
It is recommended, that based on the assessed minimal fetal risk for adequately controlled diagnostic imaging under 50 mGv, scans that are likely to provide significant diagnostic information of value to a pregnant woman should not be withheld; however, this still requires a risks and benefits discussion between a woman and her HCP.
Contrast Agents
MRI has been shown to be useful in the diagnosis of gynecological and obstetric problems during pregnancy, especially in the setting of abdominal pain (appendicitis) when labor has been ruled out. MRI procedures may also sometimes require contrast agents.
Contrast agents: intravenous contrast aids in CT/MRI diagnosis by providing for visual enhancement of soft tissues and vascular structures; gadolinium and iodine-based contrast agents are the most common.
Gadolinium-based and iodinated IV contrast agents both cross the placenta, enter the fetus, and are excreted into amniotic fluid. No well-controlled studies have been completed regarding the effects on contrast agents on the fetus, therefore the risk is unknown:
An animal study published in November 2021 determined gadolinium-based contrast agents elicit uterine contractions at clinically relevant concentrations (when directly applied to the tissue).
The American College of Radiology (ACR) and ACOG do not recommend the routine use of gadolinium during pregnancy, largely due to concerns regarding the fetal thyroid.
IV iodinated contrast administration during pregnancy is recommended only when it is deemed necessary for prompt and accurate evaluation of the pregnant woman's medical condition.
Dental X-rays
Unless necessary due to significant trauma or risk of infection, HCPs will usually wait until after delivery to take dental x-rays even though most of these x-rays do not affect the abdomen or pelvic area.

If a pregnant woman and her HCP determine dental x-rays are required, the radiation risk to the fetus is considered extremely low, and many additional precautionary measures can be taken. A leaded apron should be used to shield the abdomen, a thyroid collar should be placed around the neck, and speed films should be used.
The volume of radiation that a fetus may acquire from a mother’s dental x-ray is estimated at 0.01 millirads.
The mother would need 100,000 dental X-rays for the fetus to receive just 10 mGy.
Microwave/Non-Ionizing Radiation
Heating is the main biological effect of electromagnetic fields (EMF) (i.e. a microwave oven heats up food). Currently, no adverse health effects from low level, long-term exposure have been confirmed.
The human reproductive risk of non-ionizing radiation, which includes EMF emitted from computers, laptops, microwave ovens, power lines, cellular phones, household appliances, and wireless Internet is estimated to be minimal to nonexistent.

However, several observational studies have found a potential miscarriage link with EMF exposure, but this remains very inconsistent; EMF measurements are very subjective and unreliable.
In general, miscarriage does remain one of the potential adverse health outcomes the World Health Organization has recommended to be further studied regarding EMF exposure.
A study published in February 2021 assessed EMF exposure in pregnant rats. The study indicated that the exposure to RF‐EMF (SAR of 4 W/kg for 8 h/day) during pregnancy increased cortisol (stress hormone) levels in the mother; however, the placental barrier protected the fetus from maternal stress.
Radiation Therapy Exposure
If pregnant women are exposed to an individual residing in the same household who is undergoing radiation therapy, several precautions may be required.
Radiation therapy uses high-energy waves to destroy or damage cancer cells. There are three types of radiation: external beam and temporary or permanent internal radiation. Only individuals receiving internal radiation can give off radiation for a short time.
If a loved one is receiving internal radiation in which the implant or device was left in place, pregnant women may need to avoid physically touching that individual for a few days, to include touching that individual's body fluids. If the implant or wire was removed before leaving the facility, then physical touching/contact is usually considered safe.
Pregnant women, and the individual receiving the treatment, should speak to the radiology team about all restrictions in place. The radiology team should be made aware the patient may be in close or continual contact with a pregnant woman.
Air Travel-Related Radiation
For air travel-related radiation, to include cosmic radiation and airport scanners, read here.

Action
Any pregnant woman requiring medical imaging that uses radiation should have a risks and benefits discussion with her HCP. There are numerous scenarios in which the valuable medical information that will be evident from an imaging scan may outweigh any potential risk to the fetus.
Women should talk to their HCP if they have any radiation concerns during pregnancy.
Women who work in a location in which they could be exposed to abnormal amounts of radiation (to include flight attendants) should view the resources below.
Resources
Fetal Radiation Exposure Chart by Type of Imaging Test (Canadian Medical Association Journal)
Guidelines for Diagnostic Imaging During Pregnancy and Lactation (American College of Obstetricians and Gynecologists)
Ionizing Radiation Dose Ranges Graphic (U.S. Nuclear Regulatory Commission)
Radiation and Pregnancy: A Fact Sheet for the Public (U.S. Centers for Disease Control and Prevention; 2011)
Radiation and Pregnancy: A Fact Sheet for Clinicians (U.S. Centers for Disease Control and Prevention; 2020)
Pregnant Workers who may be Occupationally Exposed to Radiation (Occupational Safety and Health Administration)