Face

Development of the face is a major milestone. The first trimester ultrasound, when most facial development is complete, finally shows the fetus with a more human-like appearance.
Development of the face is very complex, involving growths, swellings, expansions, mergers, and fusions of various structures in the same rapid time frame in early pregnancy. While genetics controls most of this process, outside factors also play a role.
Assessment of the fetal face is also more than just structural, as facial movements at specific times and under certain stimuli can “prove” healthy brain, muscle, nerve, and sensory development. Researchers are still learning about how much the face can tell us about fetal development, such as when taste occurs, the visualization of light through the uterus, or when pain may be felt.
Background
Genetic factors play the biggest role in the development of the face, especially early in pregnancy. In later stages of facial development, environmental factors (alcohol, drugs, medications) play a more increasing importance.
Development of the face includes structures such as arches, grooves, pouches, membranes, and prominences (or processes), that give rise to most components of the face through growth, enlargement, and fusion. Any disruptions during this part of development can result in various types of facial clefts or other birth defects.
More severe congenital problems tend to develop earlier in facial development (6 to 10 weeks of pregnancy); more minor problems usually develop later (10 to 14 weeks).
Face - Overview
Although the face does not formally take shape until the end of the first trimester, sizing and positioning of different facial components begins 17 to 18 days after fertilization – before most pregnancies are even recognized.
The pharyngeal apparatus develops during the 6th week of pregnancy; these structures give reason to almost all of the face and neck:
Pharyngeal arches (5 total)
Pharyngeal pouches (4 total)
Pharyngeal grooves (4 total)
Pharyngeal membranes (4 total)
At the end of 6 weeks of pregnancy, the first two pharyngeal arches give rise to individual tissue “swellings” known as facial prominences, which start to form the face.
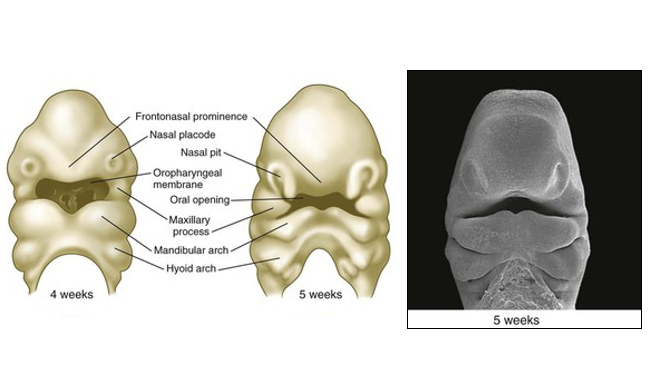
There are five prominences: the frontonasal, two maxillary, and two mandibular prominences.
These prominences grow towards the center of the face and fuse together to create the nose, mouth, lips and the front part of the palate. It is possible during these processes that the prominences do not meet correctly, which results in a structural defect of the face.
For example, the lower jaw and lower lip, formed from the two maxillary prominences, are the first parts of the face to form; an incomplete fusion of these prominences is what creates a chin dimple.
The face develops and expands rapidly between 9 and 11 weeks, giving the face a four-fold increase in length and a two-fold increase in height (little change in width).
By the 12th week of pregnancy, the nasal and maxillary processes begin to expand and fuse to form the upper lip. This development continues into the 14th week with completion of the soft palate. If the prominences do not mold together correctly, a cleft lip occurs at the boundary.
The palate separates the oral and nasal cavities. The hard palate involves the hard, bony part of the roof of the mouth, while the soft palate refers to the muscles and tissues. Cleft palate occurs when the two palatine shelves (at the roof of the mouth) fail to fuse, and therefore the mouth and nasal cavities are merged.
Cleft lip and cleft palate can occur separately, but they are also common together, despite having different origins. Cleft lip appears to be more common in males, and cleft palate occurs more often in females. In females, the palate fuses one week later than in males (around week 10).
A study published in July 2021 reviewed a total of 13,808,795 pregnancies in the United States from 1999 to 2015. A total of 10,567 primary palatoplasties (cleft palate surgery) were performed in that period of time reflecting an overall rate of 7.7 palatoplasties per 10,000 deliveries. The authors noted that this rate is decreasing, and could be a result of a lower number of women smoking during pregnancy (among other factors).
Visualization of the fetal face is possible in most ultrasound examinations beyond 12 weeks of pregnancy, and any abnormalities may be detected at this time. Additional growth of the face after this point is mostly proportion-related adjustments and correct positioning of all facial structures.
Nose
Around 7 weeks of pregnancy, nasal placodes (thickenings) develop and then sink to form nasal pits (holes/cavities). These pits are the first major development that starts to give the face a recognizable shape. The nasal cavities are plugged early in pregnancy but become unplugged around 18 weeks (read Amniotic Fluid and Respiratory Tract).

Facial development nears completion when the nose reaches its mature form and the sinuses begin to emerge.
Smallness of the nose is a common finding in newborns with trisomy 21, but is also associated with more than 40 other genetic conditions.
In one study that assessed nasal characteristics of fetuses with trisomy 21, the nasal bone was absent in 43 of 59 trisomy 21 fetuses, but in only 3 of 603 chromosomally normal fetuses.
Teeth
During the 7th week of pregnancy, a membrane above the mandibular prominence (lower jaw) starts to disintegrate to form the opening of the mouth.
Two types of teeth form in utero: “baby teeth” and permanent teeth.
Around 8 weeks of pregnancy, the dental lamina forms in the developing gums of both jaws, which eventually gives rise to 10 circular tooth buds in each jaw (upper and lower). The tooth buds for the permanent teeth begin to appear around 12 weeks. Tooth buds for the second and third permanent molars appear after birth.
Enamel is the hardest tissue in the body, and as it develops, the tooth forms into the shape of a bell. The full development of fetal tooth enamel occurs in the last two months of pregnancy and starts with the upper incisors.
Baby teeth have well developed crowns at birth, while the permanent teeth remain as buds.
As the baby teeth continue to develop after birth, they begin a continual but gradual movement toward the gum line, until they eventually “erupt” through the gum and the first tooth can be spotted. The first tooth (20 in total) can appear anytime between 6 and 24 months, and sometimes earlier. Girls usually erupt sooner than boys.
Approximately 1 in 2,000 newborns will have a tooth at birth, that will likely need removed. Although some parents may wish to keep the tooth in place, the recommendation of removal is due to the possibility the tooth could fall out and land dangerously in an infant or child’s airway. Teeth that erupt too soon are usually very loose due to immature roots.
Taste
At the end of 6 weeks of pregnancy, the tongue bud appears and is initially attached to the floor of the mouth. A failure of this tip to later detach is known as “tongue tie”.
The surface of the tongue eventually contains taste buds. The start of taste bud development is not clear, but is estimated to be between 10 and 17 weeks of pregnancy. Researchers are still learning how the taste system develops in utero, as it has only recently received increased attention in the last decade (and is mostly studied in rodents).
Regardless of the exact moment taste buds develop, they are presumed to be functional by mid-pregnancy. It is currently believed the flavor of amniotic fluid changes based on the food choices of the mother, which can then be detected by the fetus after this point.
It is theorized that experiences with certain flavors that pass through amniotic fluid (and breast milk) can lead to heightened preferences for these flavors after birth. Further, infants have been documented to orient toward the odor of their own amniotic fluid.
Additionally, in utero, fetal facial responses can be observed from bitter tasting substances at 28 to 30 weeks of pregnancy, indicating the pathways between taste buds and facial muscles are established by this point in pregnancy.
Facial Movement
Facial muscles start to develop between 5 and 10 weeks of pregnancy and are completely formed by 16 weeks. However, some researchers believe it is unclear when the ability to purposefully make facial expressions begins, as this also involves brain and nerve development.
However, fetuses do show various facial expressions such as blinking, yawning, sucking, mouthing, scowling, smiling, and sticking out the tongue, and these expressions get much more coordinated and expressive as pregnancy progresses.

Facial movements seen during ultrasound screenings are indicative of healthy brain development. The fetal face can mirror brain function and development during different stages in utero. The face can “prove” that the facial muscles and brain connections to control them, are working properly – especially when the face responds to certain stimuli (light, sound) outside the uterus.
Action
It is important that women avoid drinking alcohol, quit smoking, and tell their HCP of any medications they used either just prior to pregnancy or during the first few weeks. While not all medications cause problems during pregnancy, some medications may need to be stopped or changed as soon as a woman learns she is pregnant.
Women should also explain their family, medical, and obstetric histories during the first prenatal appointment, but ideally during genetic screening or a pre-conception appointment.
Women who have any questions or concerns regarding their baby's facial development should speak with their HCP or a genetic counselor.
Resources
A photo of a 6 to 7 week old embryo with labeled facial prominences can be viewed here (microscopic image); (UNSW Australia/Embryology)
Face Development Video Clip (7 seconds) (UNSW Australia/Embryology)