Arms, Hands, Legs, and Feet

The development of fetal limbs begins around 5 to 6 weeks of pregnancy. The upper limbs are always a few days ahead of lower limb development, to include legs, feet, and toes, but can all be well observed via ultrasound by 10 weeks of pregnancy.
Women can observe their baby moving their arms, legs, hands, and feet during the first-trimester ultrasound scan, around 12 to 14 weeks, which further improves by the mid-pregnancy scan, around 18 to 22 weeks.
Women can begin feeling these movements around 18 to 23 weeks in a first pregnancy, and as early as 16 weeks in a subsequent pregnancy.
At this time, there are no specific nutrient requirements or supplements that can help prevent limb defects. However, there are medications women should avoid; therefore women should make sure they inform their HCP of all medications they are currently taking or have recently taken.
Women should read below to learn more detailed information about limb development.
Background
The development of arms and legs starts after the basic body shape has already formed. Limbs cannot grow just anywhere on the body; limb fields are generated in very specific locations; however, the initial positioning of the limbs is much higher than what will end up being their final location.
Limb Development
The critical period of limb development is from 5 to 10 weeks of pregnancy. The upper limbs, to include hands and fingers, are about 2 to 5 days ahead of leg, foot, and toe development.
The upper limb buds appear at 5 weeks, and the lower limb buds appear at end of the 6th week.
Between 6 and 7 weeks of pregnancy, the hand (and foot) plates can be seen, with small constrictions that will eventually form the wrists. Mini fingers begin to form, and nerves are migrating to the limbs. The forearm and shoulder can also be seen. A few days after their development, the thigh, leg, and foot are also very distinct.
During 8 weeks of pregnancy, fingers are a bit more defined, but still webbed. Beginning at 8 to 10 weeks, the limbs lower slightly along the body to their final locations.
This image contains triggers for: Real Embryo
You control trigger warnings in your account settings.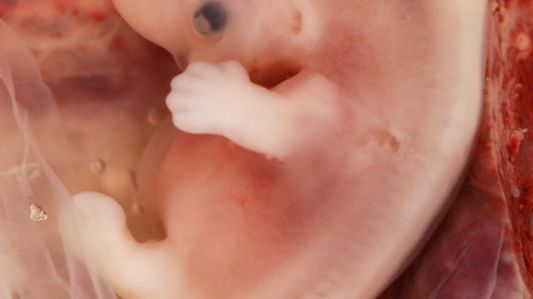
During week 9, the limbs can bend at the elbow and fingers are slightly less webbed; toes are much more visible.
The “extra” cells between the future fingers and toes are removed by programmed cell death called apoptosis. These cells essentially die which leads to finger/toe separation from what were once “paddle-like".
During week 10, fingers and toes are both very distinct and separated.

Ossification (bone formation) of limbs begins at 10 weeks of pregnancy and starts to make demands on the mother’s supply of calcium. Primary ossification centers develop in all the long bones of the limbs by the 12th week.
By the end of 14 weeks of pregnancy, the upper limbs have almost reached their final lengths (relative to the rest of the fetal body) but the lower limbs are still slightly shorter than their relative length.
To get knees and elbows pointed correctly by birth, the upper and lower limbs rotate in opposite directions and to different degrees.

Limb Movements
Fetal movements are commonly described as flutters, bubbles popping, hiccups, gentle kicks, puffs of air, rolling, butterflies, stretching, turning, and swishes.
Fetal activity can be observed as early as 8 to 10 weeks of pregnancy by ultrasound but is usually not felt – by first-time mothers – until around 18 to 23 weeks (known as “quickening”). Women who have previously felt fetal movements may feel movement as early as 16 weeks in subsequent pregnancies.
Read Fetal Movement for more detail.

Limb Defects
Major limb defects appear in about 1 in 500 to 6 in 10,000 live births.
The causes of limb abnormalities are very complex, involving single gene disorders (most common), chromosomal abnormalities, intrauterine factors, vascular events, disease, and drug/chemical exposure. In many cases involving limb abnormalities, the causes remain unknown.
Vitamin A (retinoic acid) is crucial for the development of limbs, as using certain drugs that block the synthesis of retinoic acid prevent limbs from forming. However, retinoic acid is also a known teratogen, especially when used as a treatment for certain conditions.
Note: All the vitamin A women need during pregnancy can be acquired through a regular, varied diet and prenatal vitamins. Any woman taking retinoic acid for acne treatment or any other condition needs to call her HCP immediately.
Limb deformities can be hard to track when there is no obvious associated factor.
An apparent uptick in arm deformities was reported in Germany and France in 2018 and 2019, but no official cause was determined, with officials citing the difficulty in tracking theses types of cases across regions/countries.
Action
Women who have any questions or concerns regarding their babies' limb development need to have a discussion with their HCP.
There is no need to take additional supplements during pregnancy to prevent limb defects; however, women do need to avoid taking certain medications during pregnancy. Women should keep track and tell their HCP at their first prenatal appointment (or ideally, before) all medications they have taken recently or are currently taking.
Resources
Limb Development (UNSW Australia, Dr. Mark Hill)